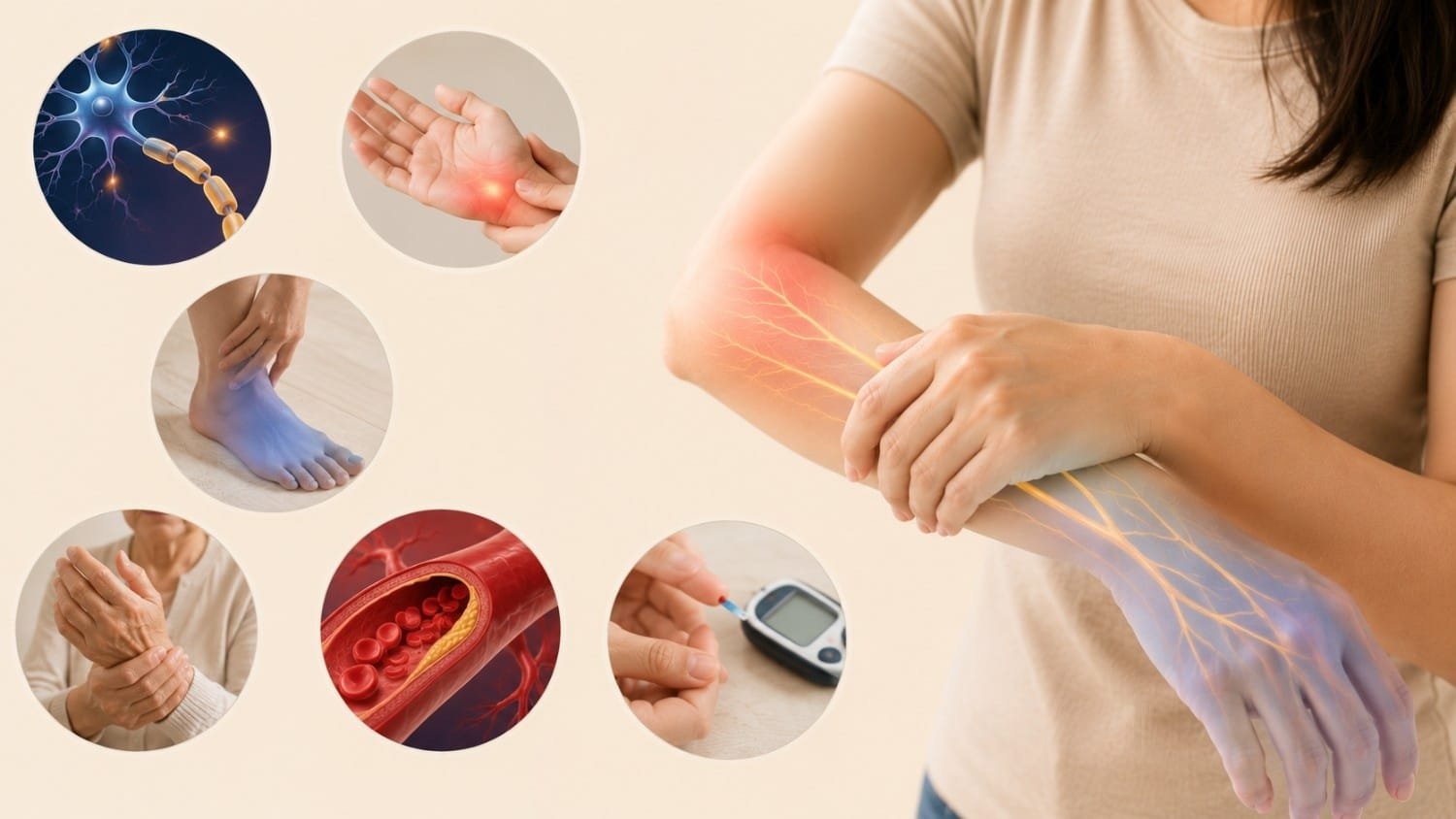
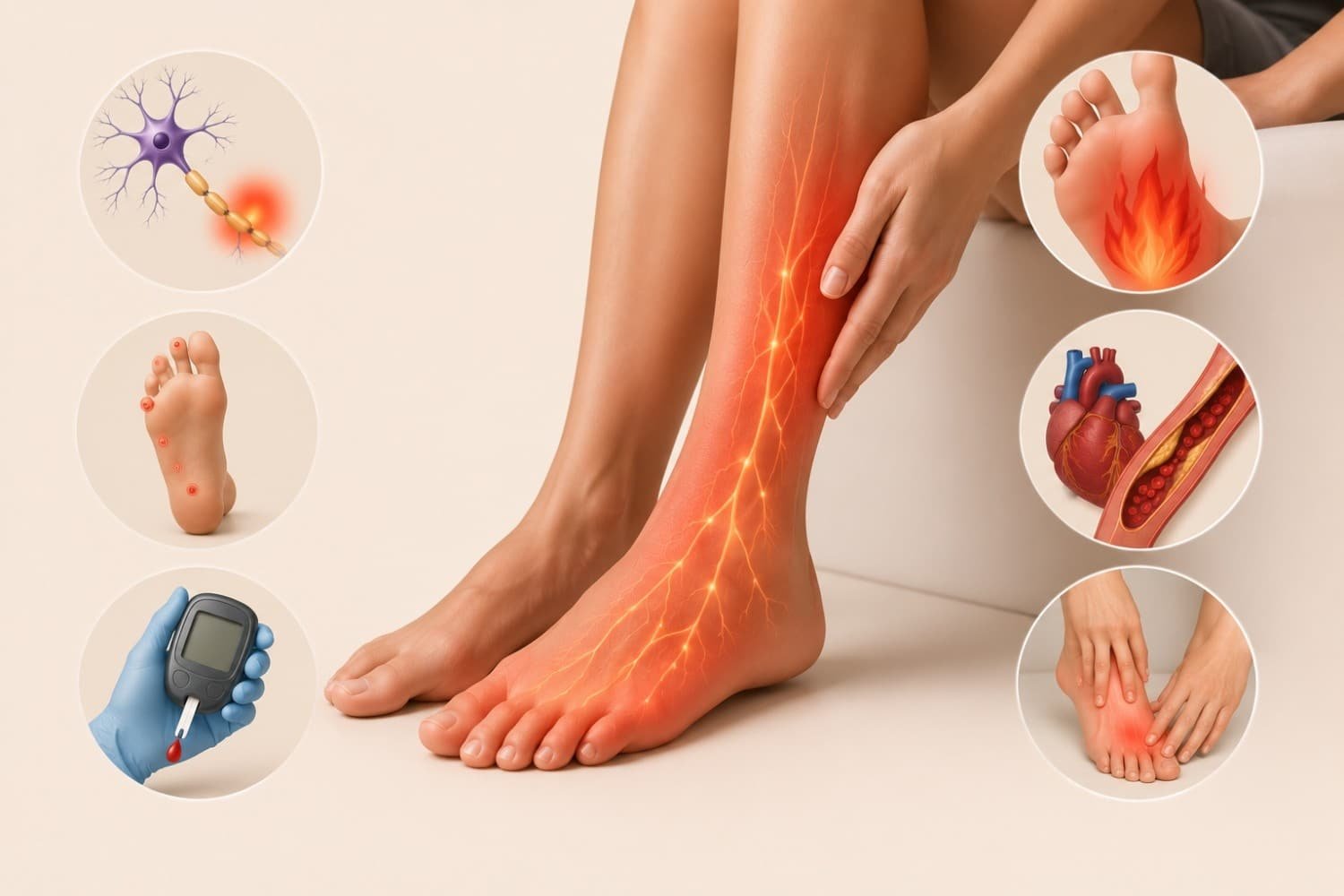
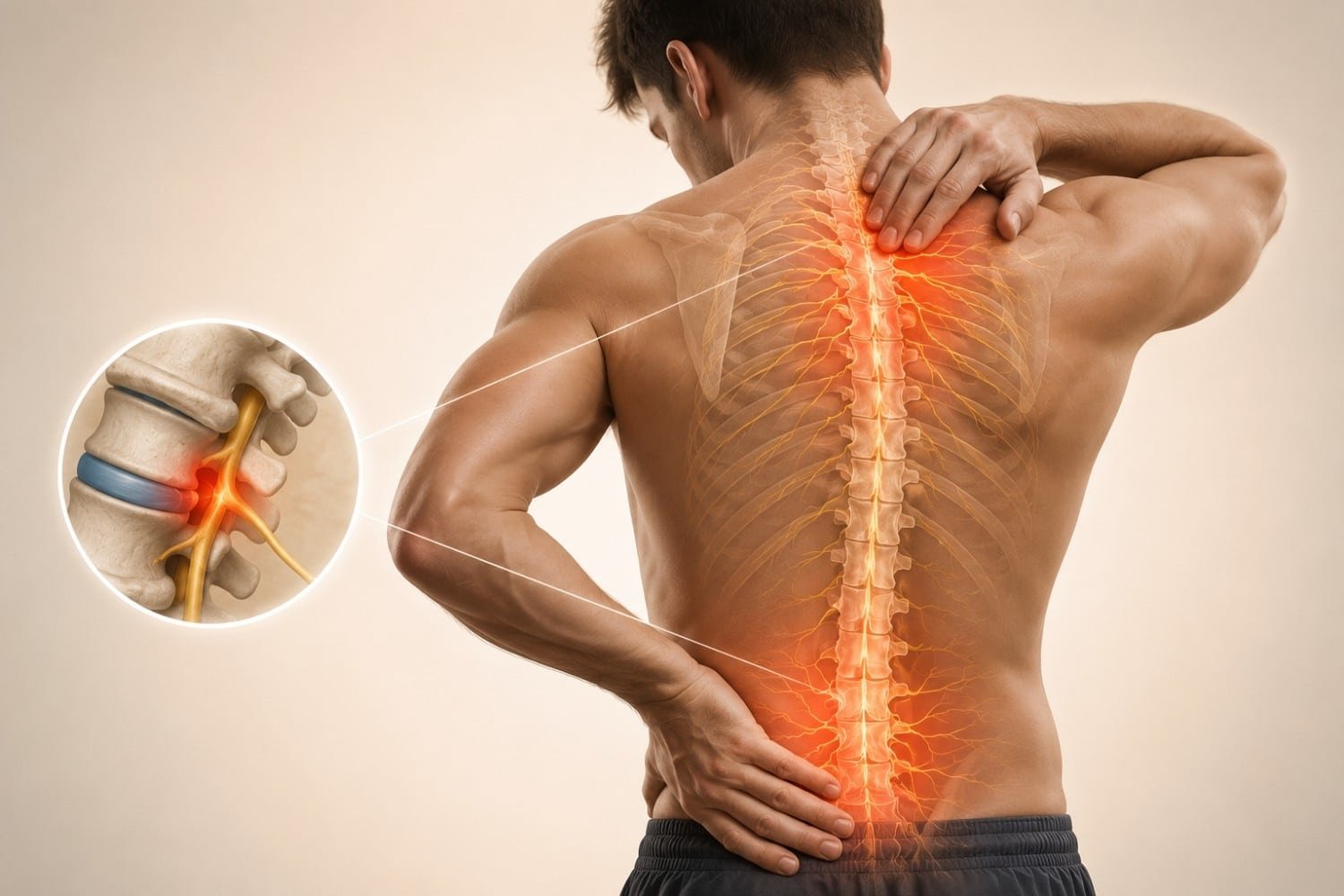
I’ve been writing about neurological health for over a decade, and if there’s one thing I’ve learned, it’s that losing sensation in any part of your body is genuinely unsettling. That tingling in your fingers, the numbness in your feet, or that strange “pins and needles” feeling these aren’t just minor inconveniences. They can signal something deeper happening with your nervous system. In this article, I want to break down what loss of sensation actually means, why it happens, what different types look like, and most importantly, what you can do about it.
What Actually Happens When You Lose Sensation
When I talk about loss of sensation, I’m referring to any reduction or complete absence of your ability to feel touch, temperature, pain, or vibration in a part of your body. Your nervous system is essentially the electrical wiring of your body it carries signals from your skin, muscles, and organs to your brain, which then interprets these signals as sensations.
This entire system can break down at several points. Your peripheral nerves (the ones extending to your limbs), your spinal cord, or even your brain itself can develop problems that interrupt these signals. The result? You either feel less than normal, nothing at all, or sometimes you feel things that aren’t actually there (like burning or tingling without any physical cause).
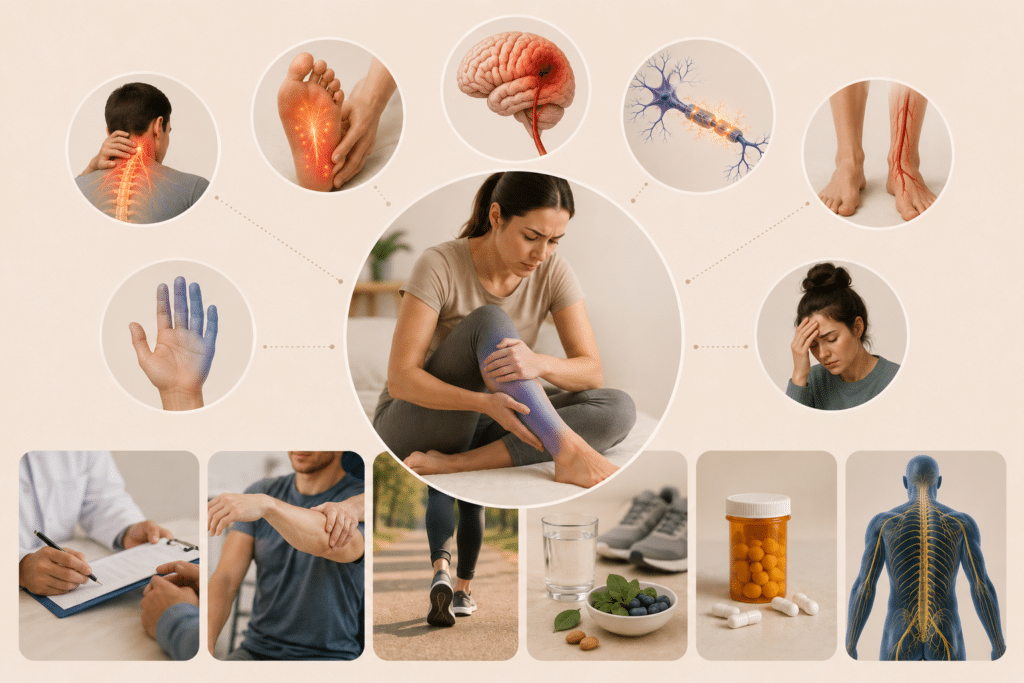
Common Causes of Sensory Loss
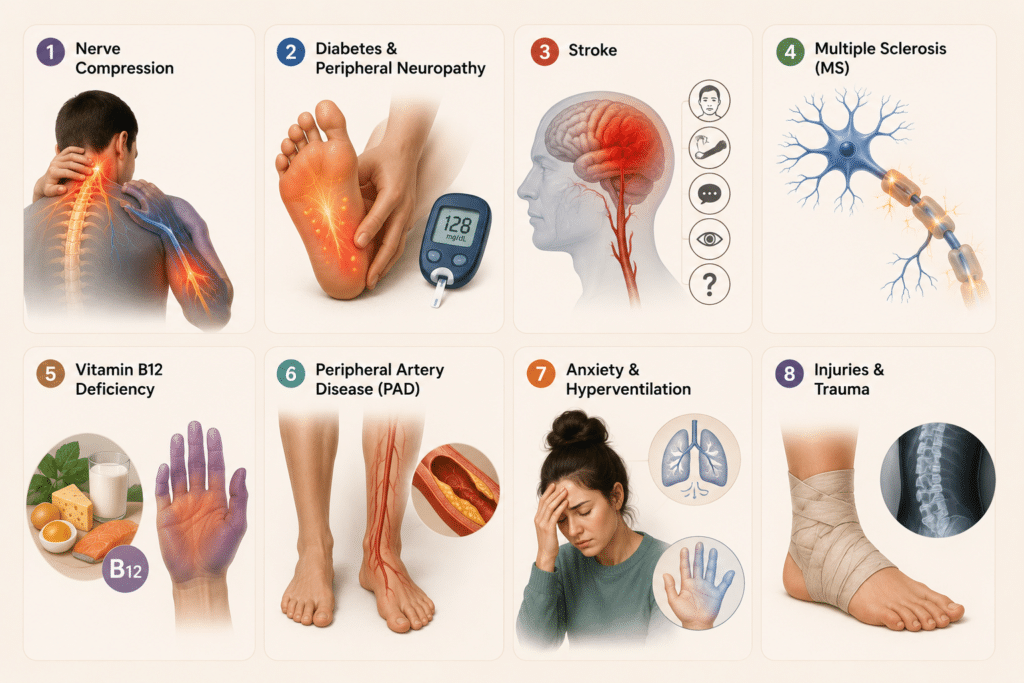
After years of researching this topic, I’ve found that loss of sensation typically stems from several key causes. Understanding where the problem originates helps determine how serious it might be.
Nerve Compression
Nerve compression is probably the most common cause I see in everyday scenarios. Think about when your foot “falls asleep” after sitting in one position too long—that’s your nerve being compressed. Carpal tunnel syndrome is another classic example, where the median nerve in your wrist gets squeezed, causing numbness in your hand and fingers. Most compression-related numbness is temporary and resolves once you change position or address the underlying issue.
Diabetes
Diabetes is another major culprit. High blood sugar over time damages small blood vessels that supply oxygen to your nerves, particularly in the feet and hands. This diabetic neuropathy affects millions of people and represents one of the most prevalent causes of chronic sensory loss. If you have diabetes and notice increasing numbness, that’s something you need to discuss with your doctor promptly.
Vitamin Deficiencies
Vitamin deficiencies, especially B12 and B6 deficiencies, can also cause significant sensory problems. Your nerve health depends on these vitamins, and when you’re low, you might experience burning, tingling, or numbness that typically starts in your hands and feet.
Nerve Injuries
Nerve injuries from accidents, surgeries, or trauma can sever or damage peripheral nerves. The recovery from such injuries varies widely—some people recover fully within months, while others may have permanent changes.
Autoimmune Conditions
Autoimmune conditions like multiple sclerosis, Guillain-Barré syndrome, or lupus can attack the nervous system, causing sensory loss that comes and goes or progressively worsens. These conditions often require specialized neurological care.
Stroke and Brain Injuries
Stroke and brain injuries affect the central nervous system and can cause sensory loss on one side of the body, depending on where the brain damage occurred.
Infections
Certain infections including Lyme disease, shingles, and HIV can lead to nerve damage and subsequent sensory loss.
Types of Loss of Sensation
Medical professionals categorize sensory loss in several ways, and understanding these distinctions helps with diagnosis and treatment.
Paresthesia refers to that “pins and needles” feeling or tingling sensation. It’s often temporary—like when your limb falls asleep but can become chronic with certain conditions. Many people describe it as a crawling sensation or a feeling of “pins” under the skin.
Anesthesia is the complete absence of sensation in an area. This is more serious and can indicate significant nerve damage. If you can’t feel anything in a particular spot, especially after trauma, seek medical attention.
Hypesthesia describes reduced sensation, where you can feel something but not as clearly as you should. This often accompanies conditions like diabetic neuropathy and progresses gradually.
Dysesthesia is an unpleasant, painful sensation that doesn’t match the actual stimulus—your brain is interpreting normal touch signals as painful or burning. This is common in conditions like multiple sclerosis and can be quite debilitating.
Hyperesthesia is the opposite increased sensitivity where normal touch feels exaggerated or painful. This occurs in conditions like complex regional pain syndrome.
Nociceptive pain loss means you can’t feel pain normally, which is actually dangerous because pain serves as your body’s warning system. People with this condition can injure themselves without realizing it, particularly in their extremities.
Recovery Pathways and Treatment Options
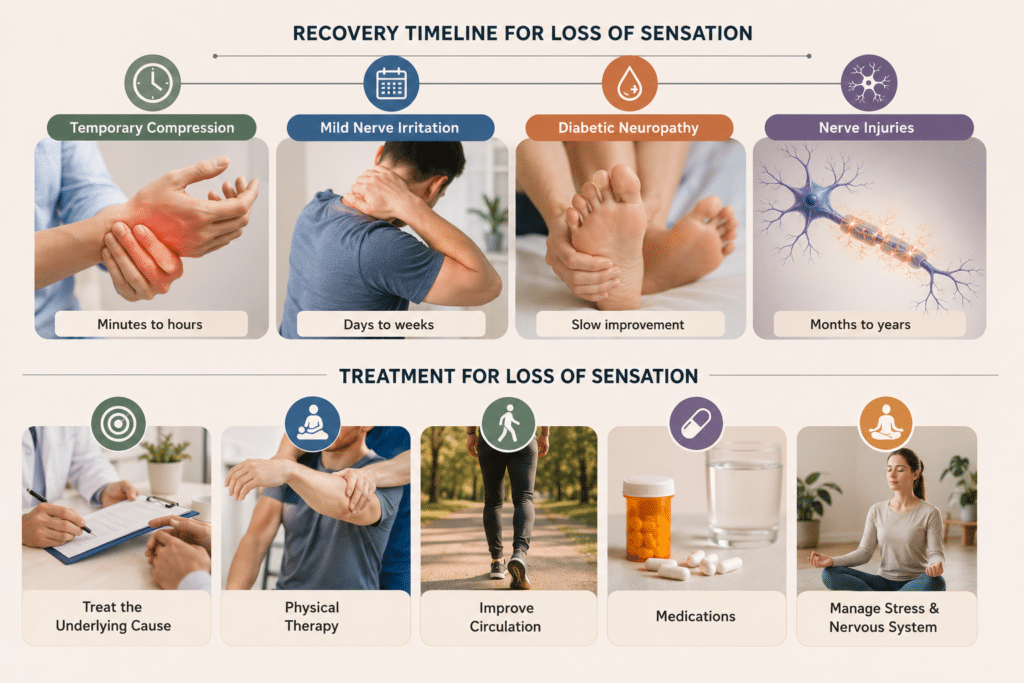
When it comes to recovering sensation, I’ve learned that outcomes depend heavily on what’s causing the loss and how quickly you address it.
For temporary compression-related numbness, simply removing the pressure usually works. Change your position, shake out your limbs, and give it a few minutes. If you’re dealing with chronic compression—like carpal tunnel splinting, physical therapy, or sometimes surgery provides relief.
For diabetic neuropathy, the key is managing your blood sugar effectively. Studies consistently show that tight glucose control slows nerve damage progression. Beyond that, certain medications, including gabapentin and pregabalin, can help manage symptoms.
If vitamin deficiency is the cause, supplementation often leads to improvement, though recovery can take several months. B12 injections are particularly effective for severe deficiencies, and I’ve seen patients make remarkable comebacks with proper treatment.
Nerve injuries are trickier. Peripheral nerves can regenerate at about one inch per month, but this depends on the severity of the injury and how far the nerve needs to regrow. Surgical repair, physical therapy, and sometimes electrical stimulation help promote nerve regeneration.
For autoimmune conditions affecting sensation, treating the underlying condition is essential. Disease-modifying therapies, corticosteroids, and other immunosuppressants may slow progression and sometimes allow partial recovery.
When to Seek Professional Help
I’ve seen too many people dismiss persistent numbness as “nothing serious.” Here’s my honest advice—seek medical evaluation if your numbness lasts more than a few days, spreads progressively, affects both sides of your body, follows an injury, is accompanied by weakness or difficulty moving, affects your face or involves speech changes, or causes bladder or bowel problems.
These could indicate more serious neurological issues requiring prompt attention.
Practical Steps You Can Take Today
Beyond medical treatment, certain lifestyle changes support nerve health. Maintain stable blood sugar if you’re diabetic, ensure adequate vitamin intake through diet or supplements, avoid smoking (it constricts blood vessels and impairs circulation), exercise regularly to improve blood flow to extremities, and protect your hands and feet from extreme temperatures and injury since you might not feel damage happening.
Frequently Asked Questions
Common causes include nerve compression, diabetes, stroke, vitamin deficiencies, circulation problems, and neurological disorders.
Yes. Anxiety and hyperventilation can temporarily alter circulation and nerve sensitivity, leading to numbness or tingling.
Recovery depends on the cause. Mild compression may improve within hours, while nerve injuries can take months.
Seek medical attention if numbness appears suddenly, worsens, spreads, or occurs with weakness, speech problems, or balance issues.
Final Thoughts
Loss of sensation can feel unsettling because it reminds us how much we rely on our nervous system every second without even thinking about it.
Sometimes numbness is temporary and harmless. Other times, it’s an early warning sign your body genuinely needs you to notice.
The key is paying attention to patterns instead of brushing symptoms aside for weeks or months.
And honestly, if part of your skin feels like it quietly disconnected from the group chat, it’s probably worth figuring out why.