A few summers ago, I woke up with a strange burning sensation on my left thigh. No rash, no redness, no insect bite just this hot, prickly feeling that wouldn’t go away. I assumed it was the weather. Spoiler: it wasn’t.
After two weeks of ignoring it like a true champion of bad decisions, I finally saw a doctor. Turns out, it was a minor nerve compression issue that had a proper medical name and a proper fix. That experience taught me something important: a burning sensation on skin is rarely “just nothing.”
In this guide, I’ll walk you through what causes it, when to worry, and what genuinely helps. Everything here is based on real medical understanding, not internet folklore.
What Is a Burning Sensation on Skin?
A burning sensation on skin is exactly what it sounds like — a feeling of heat, stinging, or scalding without an actual external source. Sometimes it comes with redness or rash, and sometimes it shows up out of nowhere on completely normal-looking skin.
Doctors call this dysesthesia when it’s nerve-related, and it falls under the broader category of paresthesia. It can affect any part of the body — face, arms, legs, back, feet — and it can last seconds, hours, or even weeks depending on the cause.
What makes burning sensations confusing is how varied they feel. Some people describe it as sunburn under the skin, others as tiny electric shocks, and a few as a slow, dull heat that won’t quit.
Burning Sensation on Skin Without Rash: Why It Happens
This is one of the most searched and misunderstood symptoms. When skin burns but looks completely fine, it’s usually a nerve issue rather than a skin issue.
Here’s the simple logic: skin problems usually show themselves visually. Nerve problems often don’t. So if the burning has no visible cause, your nervous system is likely the one sending mixed signals.
Common reasons include nerve compression, vitamin deficiencies, diabetes, anxiety, shingles in its early stage, or side effects from medications. We’ll get into each of these in detail below.
Common Causes of Burning Sensation on Skin
I’ve broken these down into three clear groups: nerve-related, skin-related, and infection-related. This makes diagnosis easier to understand, even before you see a doctor.
Nerve-Related Causes
1. Peripheral Neuropathy
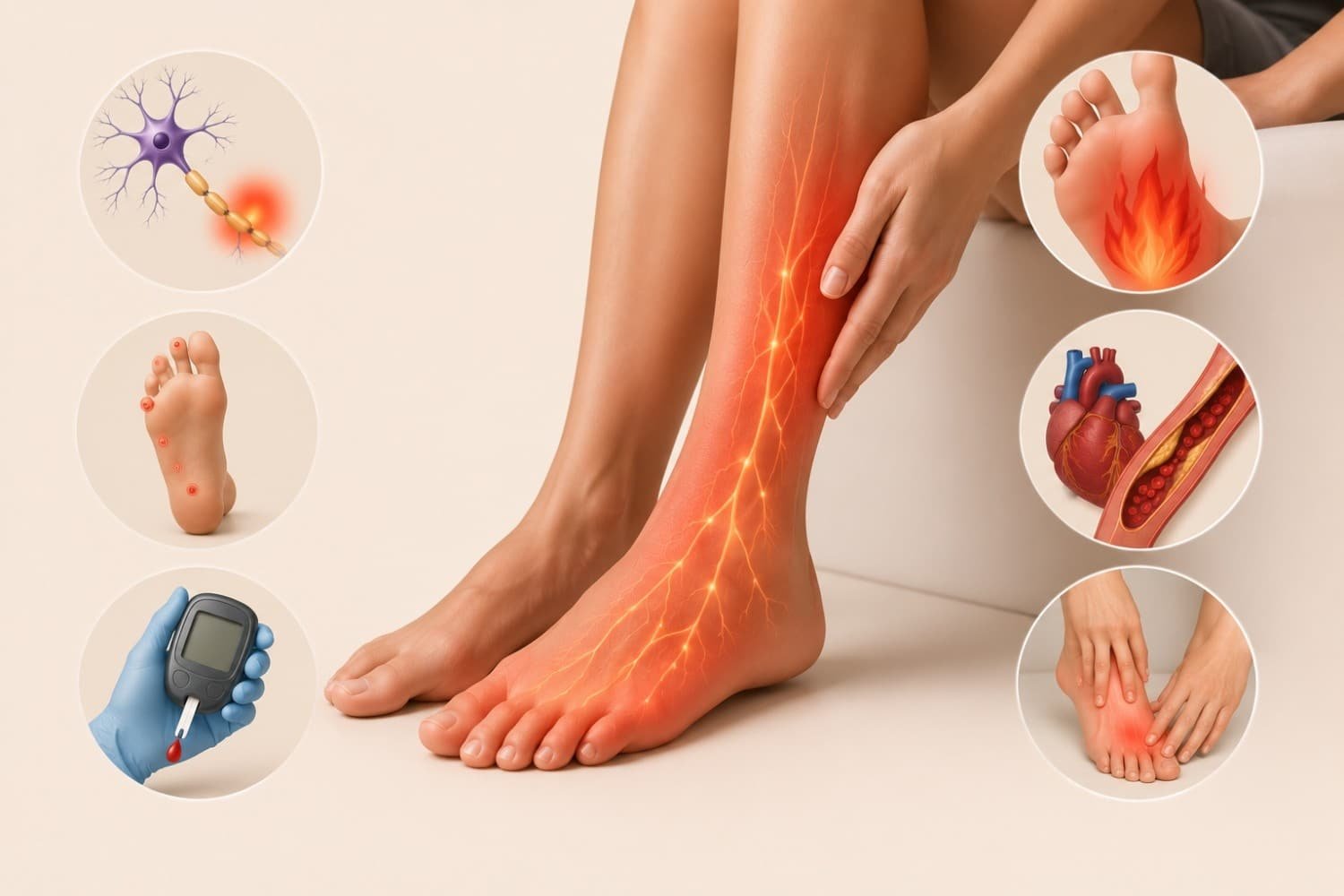
This is one of the most common causes I’ve come across. The peripheral nerves get damaged due to diabetes, vitamin deficiencies, alcohol use, or chemotherapy, and one of the earliest signs is burning skin — often in the feet or hands.
The American Diabetes Association lists burning sensations as a hallmark early symptom of diabetic neuropathy.
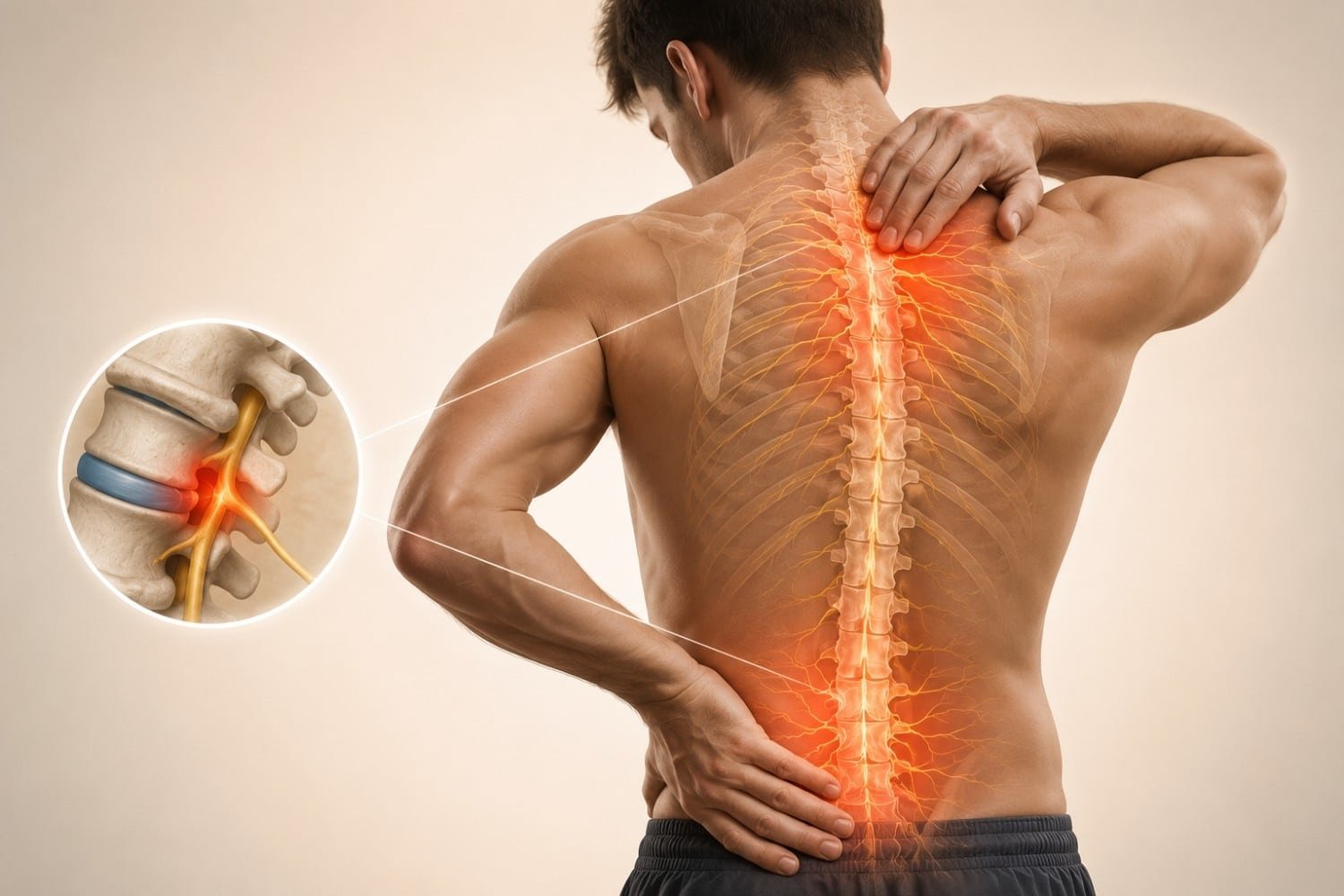
2. Pinched or Compressed Nerves
A pinched nerve in the spine, neck, or hip can cause burning sensations that travel along a specific path. Sciatica, for example, often produces burning down one leg.
I’ve had this myself after long writing sessions, and posture correction made a huge difference.
3. Shingles (Postherpetic Neuralgia)
Before shingles develops a rash, it often starts with burning, tingling, or itching on one side of the body. This pre-rash phase confuses many people because the skin still looks normal.
Even after shingles heals, some people experience long-term burning called postherpetic neuralgia.
4. Multiple Sclerosis
MS can cause burning skin sensations in random patches. It’s not the most common cause, but neurologists routinely consider it when symptoms repeat over time.
5. Anxiety and Panic Attacks
Anxiety triggers real physical changes — including burning, tingling, or heat sensations on the skin. Hyperventilation alters blood chemistry, which directly affects nerves.
I once had a panic attack so intense that my forearms felt like they were sunburnt. Nothing was wrong with my skin. Everything was wrong with my breathing.
Skin-Related Causes
6. Sunburn or Heat Damage
Even mild sun exposure can cause burning sensations hours later. Sometimes the redness is subtle, but the sensation is loud.
7. Allergic Reactions
Skincare products, detergents, perfumes, or fabrics can cause contact dermatitis. Burning is often the first symptom, even before redness shows up.
I learned this the hard way after switching face washes once. Lesson learned: always patch test.
8. Eczema and Psoriasis
Both conditions cause inflammation, dryness, and burning. Even when flare-ups look mild, the sensation can feel intense.
9. Rosacea
Rosacea causes burning, flushing, and stinging on the face — especially after spicy food, alcohol, or stress.
Infection-Related Causes
10. Fungal Infections
Athlete’s foot, ringworm, and yeast infections can cause burning before any rash becomes visible. Warm, moist areas are usually the first to react.
11. Bacterial Skin Infections
Cellulitis often starts with burning, warmth, and tenderness. Unlike fungal infections, this one needs urgent medical attention because it can spread quickly.
12. Viral Infections
Apart from shingles, infections like HIV or Lyme disease can also cause burning skin sensations as part of nerve involvement.
Burning Sensation by Body Part
Different body parts can hint at different causes. Here’s a quick breakdown based on common medical patterns.
Face
Often linked to rosacea, sun exposure, anxiety, trigeminal neuralgia, or allergic reactions. Burning on one side of the face can also indicate nerve issues.
Hands and Fingers
Carpal tunnel, diabetic neuropathy, vitamin B12 deficiency, or repetitive strain are the most likely suspects. Office workers and writers know this struggle well.
Feet and Toes
Diabetic neuropathy is the leading cause. Other reasons include alcohol-related nerve damage, fungal infections, and tight footwear.
Back
Pinched nerves, shingles, or muscle inflammation. Burning along one strip of the back, especially around the ribs, is a classic shingles warning sign.
Legs and Thighs
Meralgia paresthetica is a common but underdiagnosed cause. It’s a nerve compression issue in the upper thigh, often triggered by tight clothing, weight changes, or long hours of sitting.
This is exactly what I had during my mystery thigh-burning summer.
Scalp
Burning scalp can indicate stress, hair product reactions, scalp psoriasis, or nerve sensitivity. It’s surprisingly common and often dismissed.
Red Flags: When to See a Doctor Immediately
Most burning sensations are harmless, but some signs need quick attention. Don’t ignore these.
You should see a doctor if the burning lasts more than a few days, spreads quickly, comes with weakness or numbness, appears after a head or back injury, or includes confusion or vision changes.
Seek emergency care if burning is paired with sudden weakness on one side of the body, slurred speech, severe chest pain, difficulty breathing, or signs of a spreading skin infection like fever and warmth.
I’d rather you visit a doctor and feel mildly dramatic than miss something serious. Hospitals don’t keep score.
How Doctors Diagnose Burning Skin Sensations
The good news is that diagnosis is rarely complicated. Doctors usually start with a detailed history and physical exam.
They’ll ask when it started, where exactly it burns, whether you’ve changed any products, what makes it better or worse, and whether you have other symptoms.
From there, common tests include:
Blood tests for blood sugar, B12, thyroid function, and inflammation. Skin swabs or biopsies if infection is suspected. Nerve conduction studies for suspected neuropathy. MRI scans if nerve compression in the spine is likely.
A trustworthy doctor doesn’t guess. They test, then treat.
Treatment Options That Actually Work
Treatment depends on the cause, which is why self-medicating without diagnosis often makes things worse. Here are real, proven approaches.
Medical Treatments
For nerve-related burning, doctors often prescribe gabapentin, pregabalin, or duloxetine. For shingles, antiviral medications work best when started early. For diabetic neuropathy, blood sugar control is the foundation of recovery.
For skin conditions, topical steroids, antihistamines, or non-steroidal creams are commonly used. For infections, antifungal or antibacterial creams (or oral medication) are prescribed depending on severity.
Physical Therapy
For nerve compression issues, physiotherapy is genuinely effective. I’ve seen people fully recover from sciatica and meralgia paresthetica simply through targeted exercises and posture correction.
Lifestyle Adjustments
Stress management, hydration, sleep, and balanced nutrition matter more than people think. Burning sensations often improve when the body isn’t constantly running on stress hormones and processed food.
If you’re a smoker, quitting is one of the best things you can do for nerve health. The science is clear and consistent.

Self-Care Tips That Genuinely Help
These suggestions are simple, safe, and supported by medical reasoning.
Apply a cool (not ice-cold) compress to the affected area. Avoid hot showers, which can worsen sensitivity. Use fragrance-free moisturisers if your skin is dry. Wear loose, breathable clothing. Avoid known triggers like spicy food, alcohol, and harsh skincare.
For nerve-related burning, gentle stretching and movement help more than rest. For anxiety-related burning, deep breathing and mindfulness genuinely reduce flare-ups.
What I’d avoid: random “miracle creams,” unverified herbal patches, or DIY remedies you saw on social media. Skin is sensitive, and nerves don’t appreciate experiments.
How to Prevent Burning Skin Sensations
Prevention is more powerful than people give it credit for.
Maintain healthy blood sugar levels. Get annual blood work to catch deficiencies early. Avoid prolonged sitting or repetitive strain. Wear well-fitting shoes and clothing. Manage stress with consistent routines, not just emergency fixes.
Use sunscreen daily, even on cloudy days. UV damage is one of the easiest causes of burning skin to avoid.
And get enough sleep. Your nerves and skin both repair themselves overnight, and chronic sleep deprivation makes everything worse — including pain perception.
Frequently Asked Questions
Why does my skin burn but there’s no rash?
This usually points to a nerve issue rather than a skin issue. Common causes include neuropathy, anxiety, early-stage shingles, or vitamin deficiencies.
Can stress really cause burning sensations on the skin?
Yes. Stress and anxiety alter nerve signalling and breathing patterns, which can cause burning, tingling, or heat sensations even when nothing is wrong with the skin.
Is burning skin a sign of diabetes?
It can be. Diabetic neuropathy often starts with burning in the feet or hands, especially at night. A simple blood test can confirm or rule it out.
How long should burning skin last before I see a doctor?
If it lasts more than three to four days, recurs often, or worsens, it’s worth getting checked. Sudden or severe burning with other symptoms needs urgent care.
Can dehydration cause burning skin?
Yes, especially severe dehydration. It affects electrolyte balance and nerve signalling, which can lead to burning or tingling sensations.
Does vitamin B12 deficiency cause burning sensations?
Yes. B12 is essential for nerve health, and low levels are a well-documented cause of burning skin and tingling, particularly in older adults and vegetarians.
Can burning skin be a symptom of shingles before the rash appears?
Absolutely. Many people experience burning, itching, or tingling on one side of the body for several days before the shingles rash develops.
Final Thoughts
A burning sensation on skin can feel alarming, especially when there’s no visible cause. But in most cases, it’s your body sending a clear message usually about nerves, deficiencies, stress, or skin sensitivity.
From my own experience and everything I’ve learned, the smartest approach is simple: notice the pattern, track when it happens, and don’t dismiss it just because it isn’t “visible.”
Your skin and nerves work together as a feedback system. When that system burns, even quietly, it’s worth listening to. Early diagnosis almost always means easier treatment, and peace of mind has its own kind of value.
If you’ve been dealing with burning sensations for more than a few days, take it as a gentle reminder to check in with a qualified doctor. That single visit could save you weeks of guessing.
This article is for informational purposes only and is not a substitute for professional medical advice. Always consult a licensed healthcare provider for diagnosis and treatment.