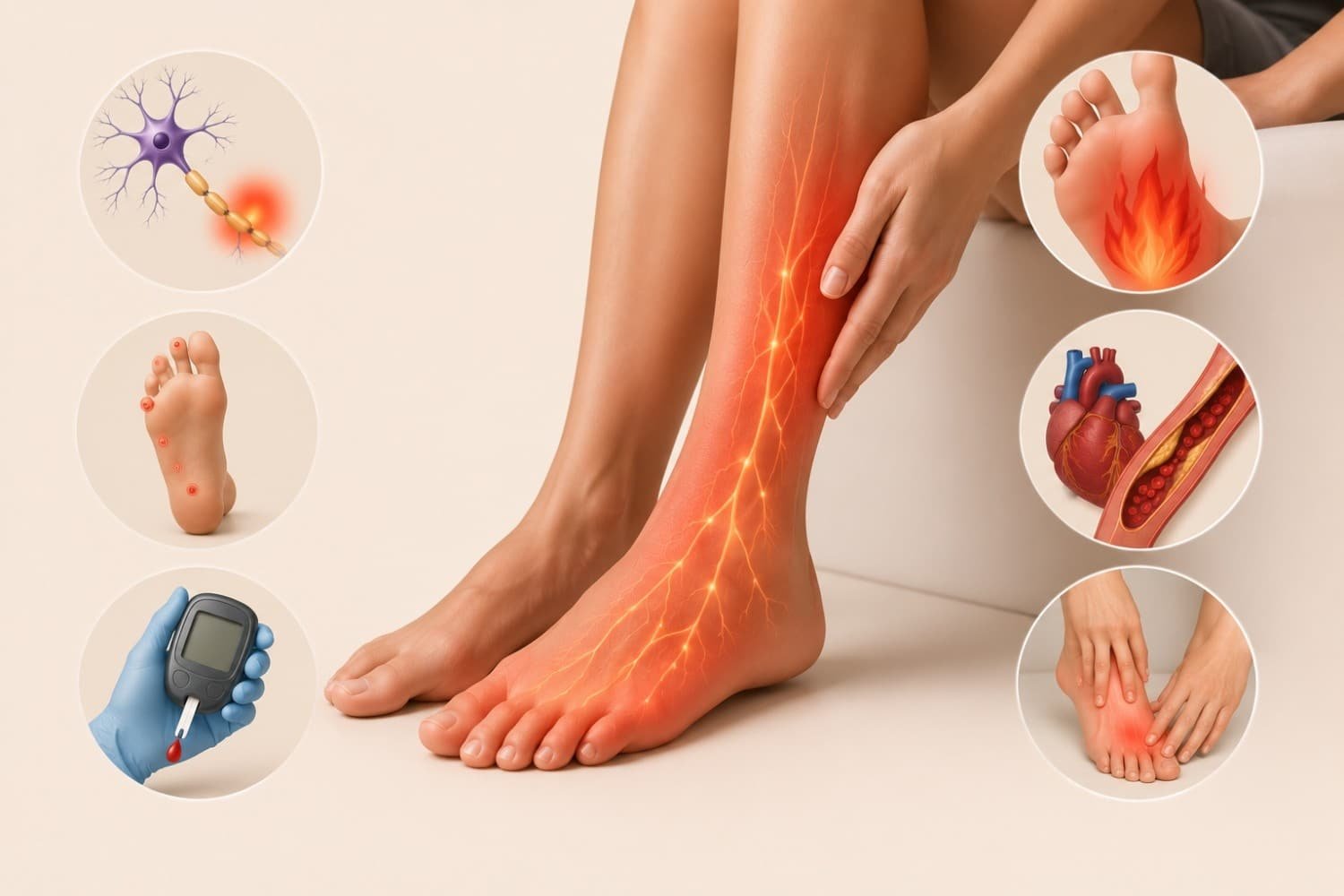
The first time I noticed something was wrong, I thought I just had bad circulation. My feet would tingle after sitting at my desk for too long, and occasionally my hands would go numb while I was driving. Like most people, I ignored it for months. That was a mistake.
Peripheral neuropathy affects millions of people worldwide, yet many don’t even know they have it until the symptoms become impossible to ignore. I learnt this the hard way after my doctor explained that the persistent tingling in my extremities wasn’t just “poor circulation” — it was my peripheral nervous system malfunctioning.
If you’re experiencing strange sensations in your feet or hands, this article will help you understand what’s happening in your body, what might be causing it, and what you can do about it.
What Is Peripheral Neuropathy
Your peripheral nervous system is the network of nerves outside your brain and spinal cord. Think of it as the electrical wiring that connects your central nervous system to the rest of your body — your limbs, organs, and everything in between.
Peripheral neuropathy occurs when these nerves become damaged or destroyed. When that happens, the communication between your central nervous system and your extremities breaks down. Messages get scrambled, delayed, or simply don’t arrive at all.
The result is a wide range of symptoms that typically start in your toes and feet, then gradually work their way up your legs. In many cases, the hands and arms are affected too. The condition can be temporary, but for many people, it becomes a permanent reality they must learn to manage.
Types of Peripheral Neuropathy
Not all neuropathy is the same. Understanding the type you have can help doctors determine the underlying cause and best treatment approach.
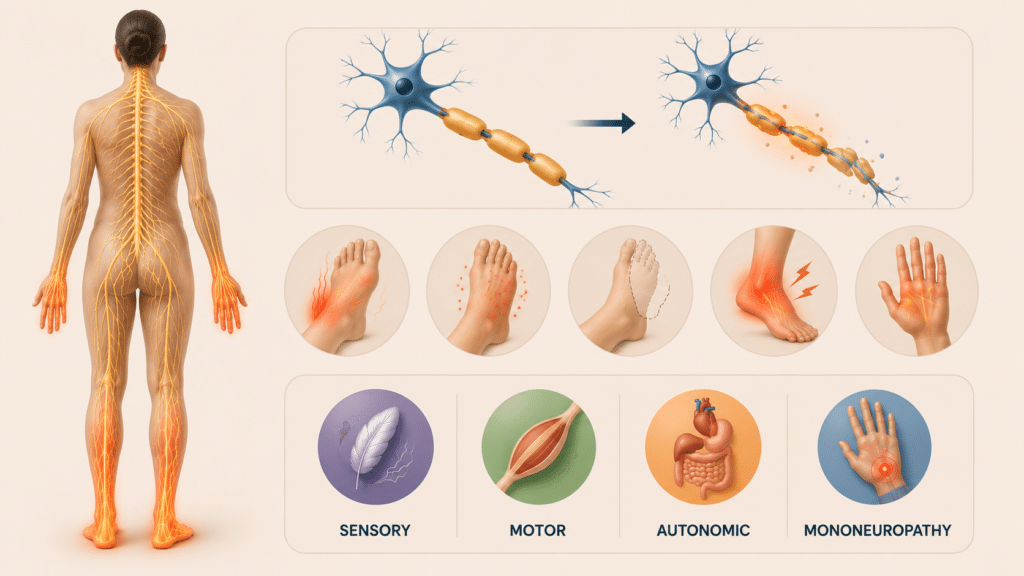
Sensory neuropathy affects the nerves that control sensation. This is the most common type and what most people think of when they hear “neuropathy”. People with sensory neuropathy might feel burning, tingling, numbness, or pain that seems to come out of nowhere.
Motor neuropathy impacts the nerves controlling muscle movement. This can lead to muscle weakness, difficulty with fine motor tasks like buttoning a shirt, and in severe cases, muscle atrophy.
Autonomic neuropathy affects the nerves controlling involuntary functions like heart rate, digestion, and blood pressure. This is more serious and can lead to problems with sweating, digestive issues, and blood pressure fluctuations.
Mononeuropathy involves damage to a single nerve. Carpal tunnel syndrome is a common example — it’s essentially a form of localised neuropathy in the wrist.
Many people have a combination of these types, which healthcare providers call “sensorimotor neuropathy”.
Common Causes of Peripheral Neuropathy
Here’s where things get interesting — and often frustrating. There are over 100 known causes of peripheral neuropathy, but some are far more common than others.
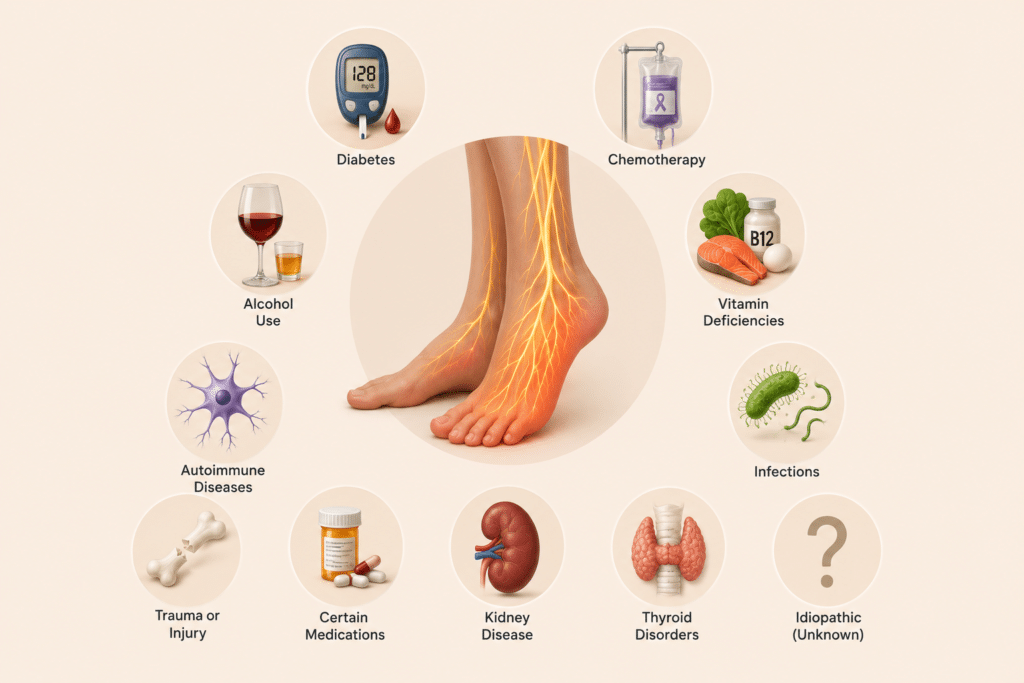
Diabetes is the leading cause of peripheral neuropathy in the United States. High blood sugar levels over time damage the small blood vessels that supply oxygen and nutrients to peripheral nerves. Studies show that up to 50% of people with diabetes will develop some form of neuropathy.
The scary part is many people don’t know they have diabetes-related nerve damage until significant damage has already occurred. That’s why regular check-ups are crucial if you have any risk factors for diabetes.
For cancer patients, chemotherapy can be a lifesaving treatment — but it often comes with a brutal side effect called chemotherapy-induced peripheral neuropathy (CIPN). The medications that kill cancer cells can also damage peripheral nerves.
CIPN affects an estimated 30-40% of people undergoing chemotherapy. The symptoms can appear during treatment and sometimes persist long after treatment ends. Some patients unfortunately experience permanent nerve damage.
Excessive alcohol consumption is a frequently overlooked cause of neuropathy. Alcohol is directly toxic to nerve tissue, and years of heavy drinking can cause what’s sometimes called “alcoholic neuropathy”.
What makes this particularly tragic is that the nerve damage from alcohol is often preventable if caught early enough. But continued drinking makes the damage irreversible.
Other common causes include vitamin deficiencies (especially B vitamins), autoimmune diseases like rheumatoid arthritis and lupus, infections including Lyme disease and shingles, trauma or injury, certain medications beyond chemotherapy, kidney disease, and thyroid disorders.
In about 30% of cases, doctors cannot determine the exact cause — this is called “idiopathic peripheral neuropathy”.
Recognizing the Symptoms
Peripheral neuropathy symptoms typically develop gradually, which is why many people dismiss early warning signs. The progression usually follows a pattern.
Early symptoms often include tingling or a “pins and needles” sensation; numbness, especially in the feet and hands; burning or sharp pain; and heightened sensitivity to touch.
Progressive symptoms as damage continues include muscle weakness, loss of balance and coordination, difficulty with fine motor tasks, and cramps and spasms.
Advanced symptoms in severe cases include significant muscle loss, difficulty walking, organ dysfunction with autonomic involvement, and chronic pain syndromes.
One thing that surprised me is symptoms often worsen at night. Many people with neuropathy find their pain and tingling becomes more intense when they’re trying to sleep, which can lead to serious sleep problems.
Diagnosis: Getting Answers
If you’re experiencing persistent symptoms, don’t wait like I did. Getting a proper diagnosis is crucial.
The diagnostic process typically involves a medical history and physical examination where your doctor will ask about your symptoms, lifestyle, medications, and family history, and they’ll test your reflexes, muscle strength, and sensation.
Nerve conduction studies measure how fast electrical signals move through your nerves, which can help determine if the nerves are functioning properly.
Electromyography (EMG) measures the electrical activity in your muscles and can show whether muscle problems are related to nerve damage.
Blood tests can identify underlying conditions like diabetes, vitamin deficiencies, or thyroid problems that might be causing neuropathy.
In some cases, MRI or CT scans can identify structural problems pressing on nerves.
Treatment Options
Here’s the honest truth: there’s no cure for most types of peripheral neuropathy. But that doesn’t mean you can’t manage the condition effectively.
The most effective treatment is often treating whatever is causing the neuropathy. If you are diabetic, getting your blood sugar under control can slow or even stop nerve damage. If a medication is causing the problem, your doctor might adjust your dosage or switch you to a different drug.
Several medications can help manage neuropathy symptoms. Gabapentin and pregabalin were originally designed for seizures but are now widely prescribed for nerve pain. Certain tricyclic antidepressants can help with nerve pain as well. Topical treatments like capsaicin cream and lidocaine patches can provide localised relief. Over-the-counter options like ibuprofen can help with mild symptoms.
Physical therapy can be incredibly valuable for maintaining strength, improving balance, and preventing falls. A good physical therapist can teach you exercises that preserve muscle function and help you adapt to balance issues.
Living With Peripheral Neuropathy: Practical Strategies
This is where I want to share what has actually helped me manage my own neuropathy — not just textbook advice, but real-world strategies.
Foot care becomes critical. If you have neuropathy in your feet, you might not feel injuries when they happen. I now inspect my feet daily for cuts, blisters, or signs of infection. I wear comfortable, well-fitting shoes – those tight stylish shoes. I used to wear are things of the past. I also never go barefoot, even at home.
Counterintuitively, gentle exercise helps. Walking, swimming, and cycling improve circulation and can actually reduce neuropathy symptoms over time. The key is starting slowly and being consistent.
I worked with a nutritionist to optimise my diet. I focus on foods rich in B vitamins, omega-3 fatty acids, and antioxidants. I’ve reduced alcohol significantly — not eliminated, but significantly reduced. This made a noticeable difference in my symptoms.
I’ll be honest — my neuropathy definitely flares up when I’m stressed or not sleeping well. Stress management techniques like meditation, deep breathing, and maintaining a consistent sleep schedule genuinely help.
There is no shame in using tools that make life easier. I use special utensils with larger grips and a pill organiser with easy-open lids, and I’ve modified my home to reduce fall risks. These are not signs of weakness — they are smart adaptations.
Frequently Asked Questions
In some cases, yes — particularly if the underlying cause is treatable like a vitamin deficiency or medication. However, in many cases, especially diabetic or chemotherapy-induced neuropathy, the damage is permanent. Early intervention offers the best chance of limiting damage.
Not always. Some people experience primarily numbness, while others have significant pain. Pain typically indicates more severe nerve damage, but numbness is not necessarily “better” — it comes with its own risks like injuries you don’t notice.
No. While risk increases with age, younger people can develop neuropathy too. Chemotherapy patients, people with autoimmune conditions, and those with certain genetic disorders can develop symptoms at any age.
Not necessarily. Most people with peripheral neuropathy never need a wheelchair. Some may benefit from a cane or walker, particularly if muscle weakness is significant. The vast majority manage with lifestyle modifications and adaptive strategies.
Absolutely. While diet will not cure neuropathy, certain nutritional approaches can slow progression and reduce symptoms. Ensuring adequate B vitamins, avoiding excess alcohol, and maintaining stable blood sugar levels are all helpful.
Final Thoughts
Peripheral neuropathy changed my life, but it did not end it. After my initial denial and delay in seeking treatment, I now manage the condition actively. I work closely with my healthcare team, I’ve made significant lifestyle adjustments, and I’ve accepted that this is now part of my life.
If you are experiencing symptoms, please don’t ignore them like I did. The earlier you get evaluated, the better your chances of addressing the underlying cause and preventing further damage. It is not about fear — it is about taking control of your health.
Living with neuropathy requires patience, adaptation, and sometimes difficult lifestyle changes. But millions of people manage this condition successfully every day. With proper medical care, practical adaptations, and a proactive mindset, you can too.