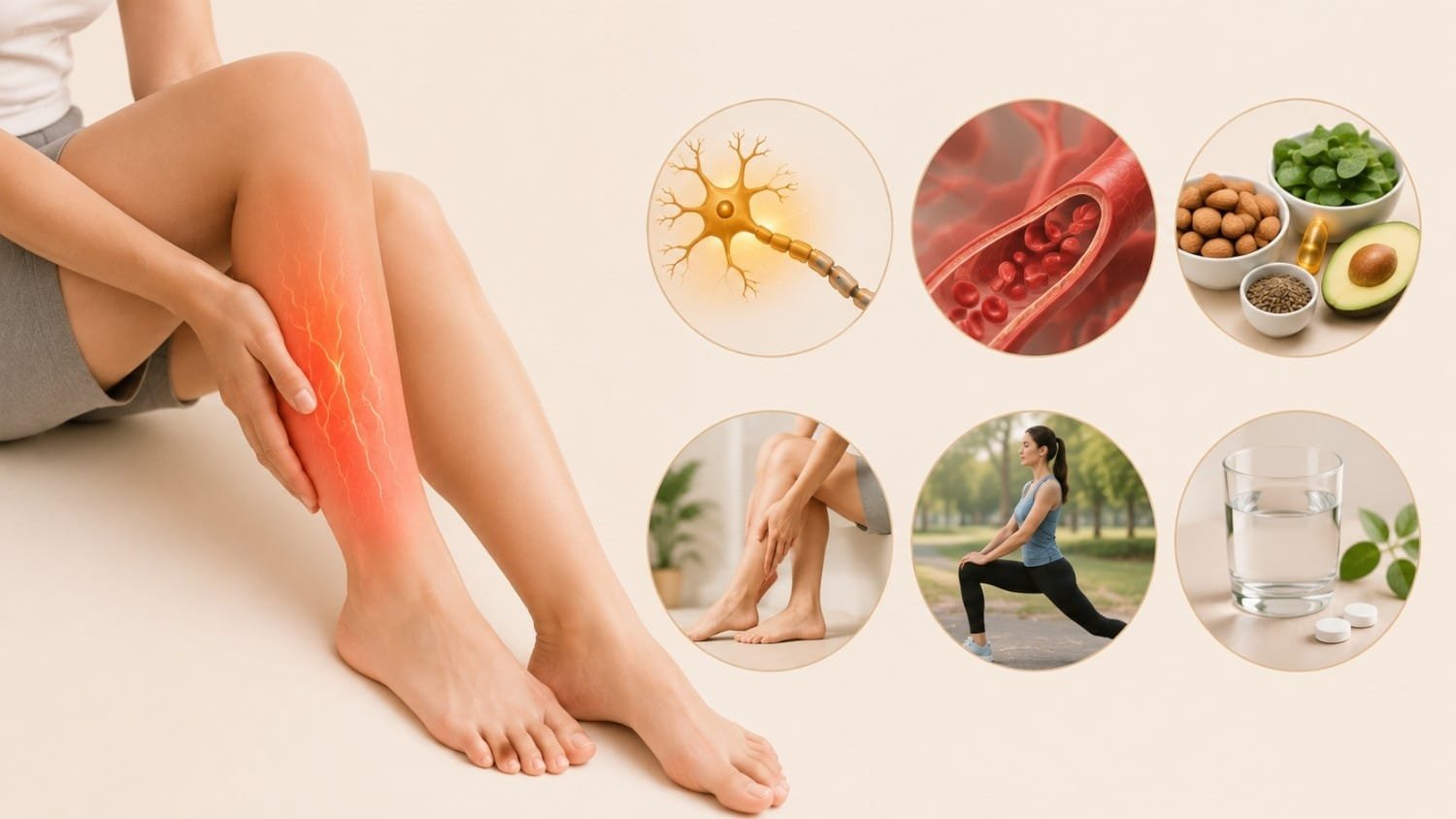
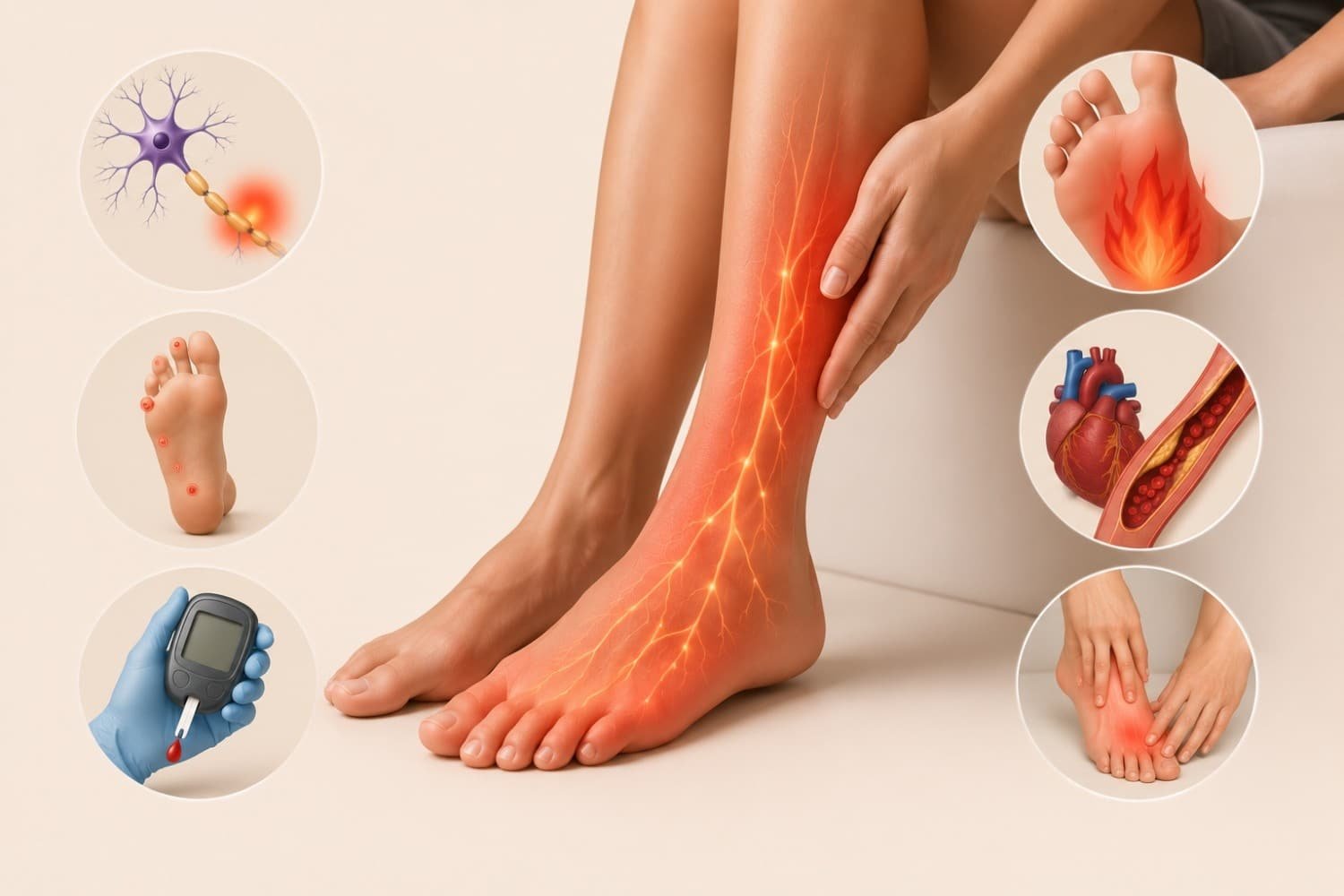
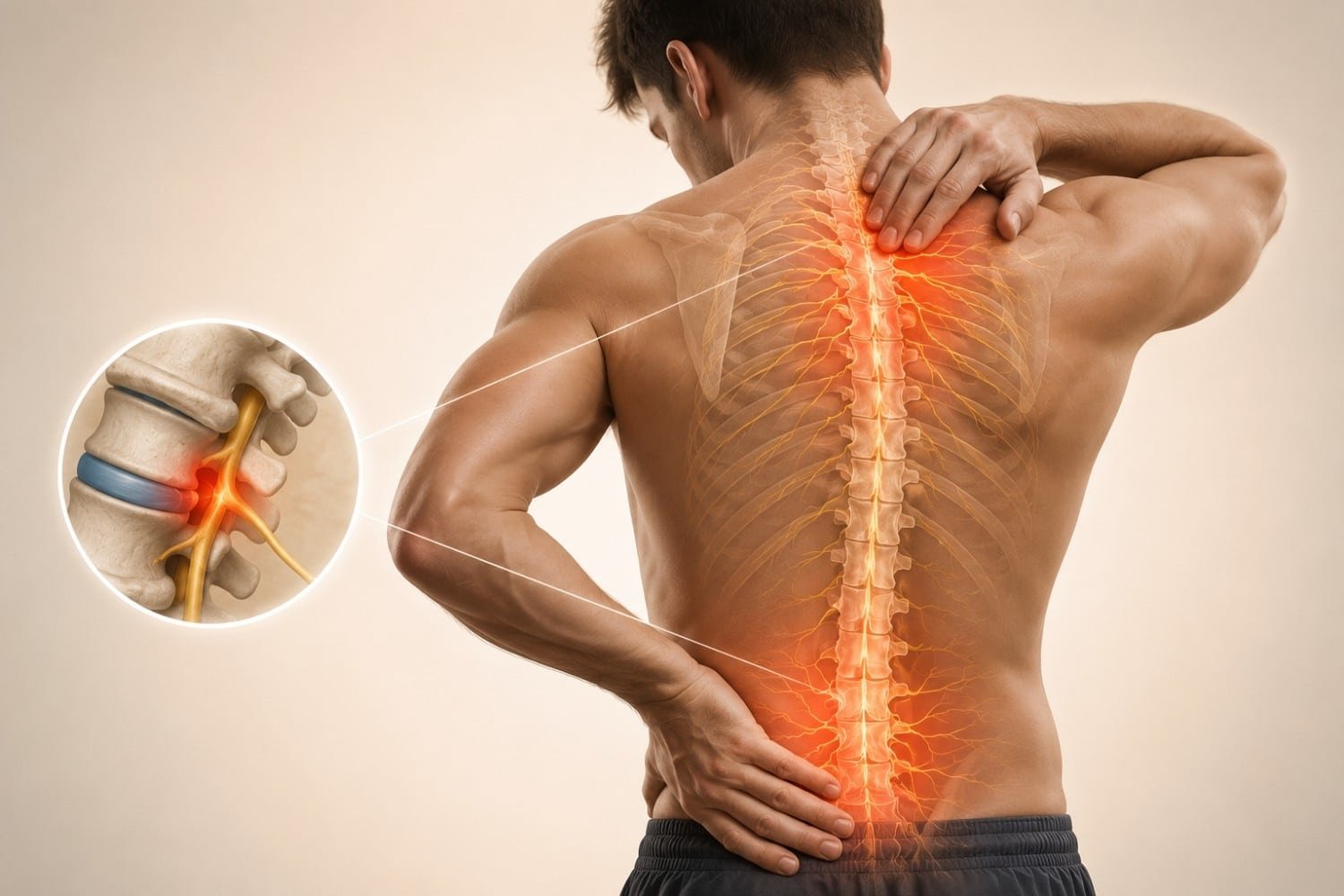
Have you ever felt like your legs were quietly catching fire from the inside, even though the room temperature was perfectly normal? I have, and the first time it happened, I genuinely checked if my pants had somehow turned into thermal wear. Spoiler: they hadn’t. My legs had just decided to host their own private heatwave.
A hot burning sensation in the legs is more common than people think, and it almost always has a real explanation behind it. In this article, I’ll walk you through what causes it, why it often gets worse at night, and how to find real relief. Everything I share here is based on credible medical sources like the Mayo Clinic, the Cleveland Clinic, the NHS, and the National Institute of Neurological Disorders and Stroke.
What a Hot Sensation in the Legs Really Means
A hot or burning sensation in the legs is a type of paraesthesia, which is the medical term for any abnormal nerve or skin sensation. Unlike tingling, this feels more like internal heat, scalding warmth, or a slow-burn discomfort.
In most cases, the heat isn’t coming from your skin. It’s coming from your nerves, blood vessels, or both. That’s why creams and cold packs only help temporarily. To actually fix the issue, you need to understand what’s happening inside the body.

Why Legs Feel Hotter Than Other Body Parts
Your legs carry a lot of nerve activity, long blood vessels, and large muscles. They’re also the body’s farthest extremities from the heart, which makes circulation issues and nerve problems show up here first.
I’ve personally noticed my own legs feeling warmer during high-stress weeks or after long sitting hours. Small lifestyle factors can produce surprisingly real sensations in the legs.
Common Causes of Hot Burning Sensation in Legs
Let me break down the most common causes, both from real-world experience and credible medical sources.
Peripheral Neuropathy
This is one of the most common causes. Peripheral neuropathy means damage to the nerves outside the brain and spinal cord, often in the legs and feet. The Cleveland Clinic recognises burning sensations as one of its earliest signs.
Common triggers include diabetes, alcohol use, chemotherapy, and certain infections. The burning is usually deep, persistent, and worse at night.
Diabetic Neuropathy
This is the most well-known type of peripheral neuropathy. Long-term high blood sugar damages tiny nerves, leading to burning, tingling, or hot sensations in the legs. The CDC reports that nearly half of people with diabetes develop this complication.
If you have diabetes and notice burning legs, please don’t ignore it. Early blood sugar control genuinely slows the damage.
Venous Insufficiency
Venous insufficiency happens when the veins in your legs struggle to send blood back to the heart. Blood pools in the lower legs, causing heat, heaviness, swelling, and aching.
You might notice your legs feel hotter after standing or sitting for long hours. Compression stockings and movement often help relieve symptoms.
Restless Leg Syndrome (RLS)
RLS is a common condition that causes uncomfortable sensations and an urge to move the legs. Many people describe the feelings as burning, crawling, tingling, or hot. Symptoms usually appear at night and disturb sleep.
The Mayo Clinic notes that RLS is often linked to iron deficiency, dopamine imbalance, or genetics. Treatment can dramatically improve quality of life.
Vitamin B12 Deficiency
Low B12 affects nerve health and is a quietly common cause of burning leg sensations. It’s especially common in vegetarians, older adults, and people on long-term acid reflux medications like omeprazole.
A simple blood test confirms it, and supplementation usually clears the symptoms.
Sciatica and Pinched Nerves
A pinched nerve in the lower back, especially the sciatic nerve, can cause burning, tingling, or hot sensations down one leg. The pain often comes with stiffness or sharp shooting discomfort.
If your hot sensation travels from the lower back through the buttock down one leg, this is likely the cause.
Peripheral Artery Disease (PAD)
PAD reduces blood flow to the legs due to narrowed arteries. Some people describe a hot or burning sensation, especially when walking, paired with cramping or fatigue.
PAD is more common in smokers, diabetics, and those with high cholesterol. It needs proper diagnosis and treatment.
Erythromelalgia
This rare but real condition causes intense burning, redness, and warmth in the legs or hands. It’s triggered by warm temperatures, exercise, or stress. Patients often describe their legs as feeling “on fire”.
If your burning is paired with redness and intense warmth, this is worth ruling out with a specialist.
Skin Conditions
Conditions like cellulitis, dermatitis, or fungal infections can cause hot, irritated skin. These often come with redness, swelling, or visible changes.
If you notice skin discolouration or warmth in a localised area, please get it checked promptly.
Hormonal Changes
Hormonal shifts during menopause, pregnancy, or thyroid issues can cause hot sensations in the legs. The North American Menopause Society lists nerve-related and temperature symptoms among the common effects of hormonal changes.
Anxiety and Stress
Anxiety can absolutely cause hot sensations in the legs. When the nervous system goes into fight-or-flight mode, blood flow shifts and nerves become hypersensitive.
I’ve personally felt hot, restless legs during stressful weeks. Once stress calmed down, the symptoms eased significantly.
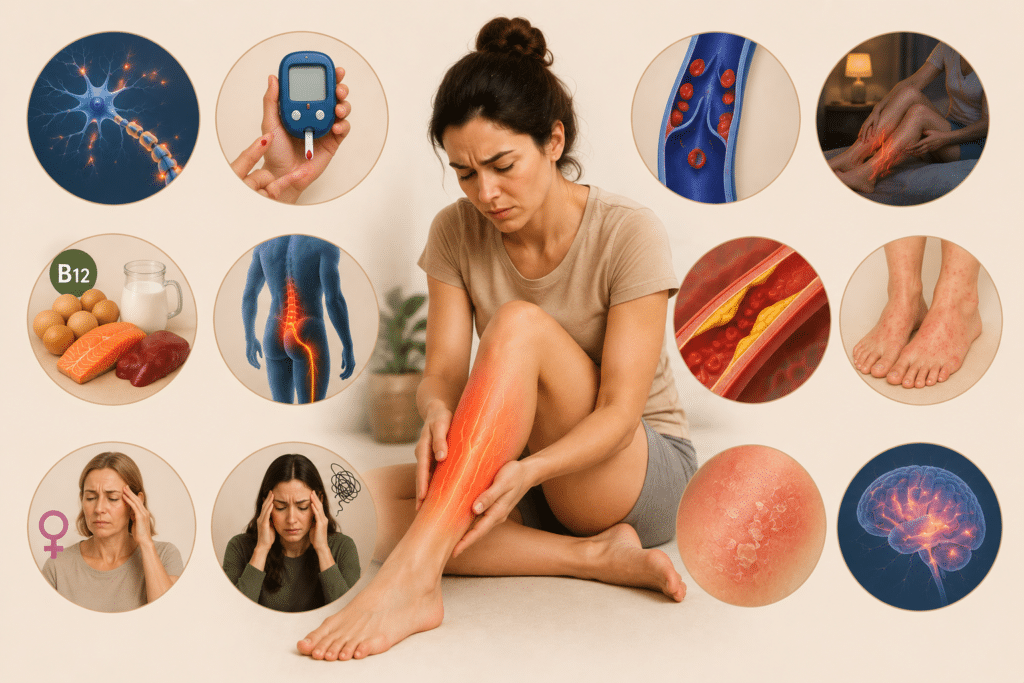
Why Hot Legs Often Feel Worse at Night
Many people with burning leg sensations notice that symptoms intensify at night. There’s a real reason for this.
At night, there are fewer distractions, body temperature changes, and the nervous system becomes more sensitive. Restless legs syndrome, neuropathy, and venous issues all flare up after lying down.
I’ve personally found that the worse my posture or hydration is during the day, the more my legs feel hot at night. Tiny daytime habits create big nighttime effects.
Day vs Night: What the Timing Tells You
If your burning sensation is mostly at night, restless legs syndrome, neuropathy, or hormonal changes are common.
If it’s after standing or sitting too long, venous insufficiency is likely involved.
If it’s after exercise, PAD or erythromelalgia may be the cause.
If it’s constant and dull, peripheral neuropathy is at the top of the list.
If it’s paired with redness and heat, skin infections or vascular issues should be evaluated.
This pattern-based approach is exactly how doctors narrow down causes during evaluation.
When Hot Legs Become a Red Flag
Most cases of hot or burning leg sensations are mild and treatable, but some need urgent attention.
Please see a doctor immediately if your hot sensation comes with the following:
- Sudden swelling in one leg
- Severe redness or skin warmth
- Difficulty walking
- Chest pain or shortness of breath (possible blood clot)
- Numbness, tingling, or weakness
- Sores that don’t heal
- Cold or discoloured limbs
Conditions like deep vein thrombosis (DVT), cellulitis, or PAD complications can become serious quickly. Trust your instincts. If something feels off, don’t wait.
How Doctors Diagnose Hot Sensation in Legs
When I finally got mine properly evaluated, the process was thorough. Diagnosing burning leg sensations isn’t a guessing game.
A standard workup includes a physical exam, blood pressure check, and blood tests for B12, blood sugar, thyroid function, and inflammation. Doppler ultrasounds check blood flow and detect venous insufficiency or PAD.
If nerve issues are suspected, nerve conduction studies and EMG help. For RLS, doctors review your symptoms and may check iron levels. The right diagnosis prevents months of guesswork.
Cooling and Relief Techniques That Actually Work
Sometimes the simplest tricks help the most. A few things I’ve personally seen work include cool foot soaks, raised legs to improve circulation, lightweight cotton clothing, and avoiding hot showers before bed.
Compression stockings from trusted brands like Mediven or Jobst help significantly with venous insufficiency. A fan at night, ventilated sheets, and breathable mattresses also reduce overheating.
Avoiding caffeine and alcohol in the evening can reduce nighttime burning, especially for those with RLS or neuropathy.
Treatment Options That Truly Help
Treatment depends entirely on the cause, but here’s what generally works in real-world cases.
Lifestyle Adjustments
For mild cases, lifestyle changes do a lot. Staying hydrated, moving regularly, stretching daily, and avoiding long sitting hours reduce nerve and circulation-related symptoms.
I started taking short walking breaks every hour, and within weeks my random burning episodes reduced sharply.
Addressing the Underlying Condition
If diabetes is the cause, blood sugar control is essential. If venous insufficiency is involved, compression therapy and movement help. RLS often responds to iron supplementation, dopamine agonists, or lifestyle changes.
In most cases, fixing the root cause solves the burning sensation for good.
Medications
Doctors may prescribe gabapentin, pregabalin, or duloxetine for nerve-related burning. NSAIDs help with inflammation. For RLS, medications like ropinirole or pramipexole are commonly used.
Always use medications under proper medical supervision.
Physical Therapy
A skilled physiotherapist can help with stretches, posture corrections, and nerve glides. This is especially helpful for sciatica, neuropathy, and circulation-related causes.
Compression Therapy
Compression stockings improve blood flow and reduce heat or heaviness in the legs. They’re widely recommended by vascular specialists for chronic venous insufficiency.
Quit Smoking and Limit Alcohol
Both worsen PAD, neuropathy, and circulation problems. Quitting genuinely changes long-term outcomes.
Surgery in Severe Cases
If conservative treatments fail, options like vein ablation, arterial bypass, or decompression surgery provide real relief in advanced cases. These are not first-line treatments but offer significant improvements when needed.

Simple Habits That Reduce Hot Sensation in Legs
A few small habits genuinely help. Stretching the calves daily, drinking enough water, avoiding tight clothing, and elevating your legs at the end of the day reduce nerve irritation and improve circulation.
If you sit for long hours, try ankle rotations, light yoga, and posture adjustments. Tiny changes create real, lasting results.
Frequently Asked Questions
It’s usually due to nerve sensitivity, neuropathy, or circulation issues. The sensation comes from inside the nerves, not the skin.
Yes. Stress and anxiety can trigger hyperventilation and nerve hypersensitivity, which sometimes produce burning sensations.
Brief, occasional warmth is usually harmless. Worry only when it’s persistent, painful, or comes with swelling, weakness, or skin changes.
Sudden swelling, severe redness, breathing difficulty, or pain in one leg can indicate a blood clot or infection. Seek medical care immediately.
Final Thoughts
A hot burning sensation in the legs may seem like a minor annoyance, but it often signals something specific. From neuropathy and venous issues to RLS and lifestyle factors, the causes are varied, and so are the treatments.
If your legs keep feeling like they’re hosting their own private summer, don’t ignore it and don’t panic either. Track the patterns, fix the basics, and consult a qualified doctor when needed. Your legs carry you through every day. The kindest thing you can do is help them stay cool, calm, and well taken care of.