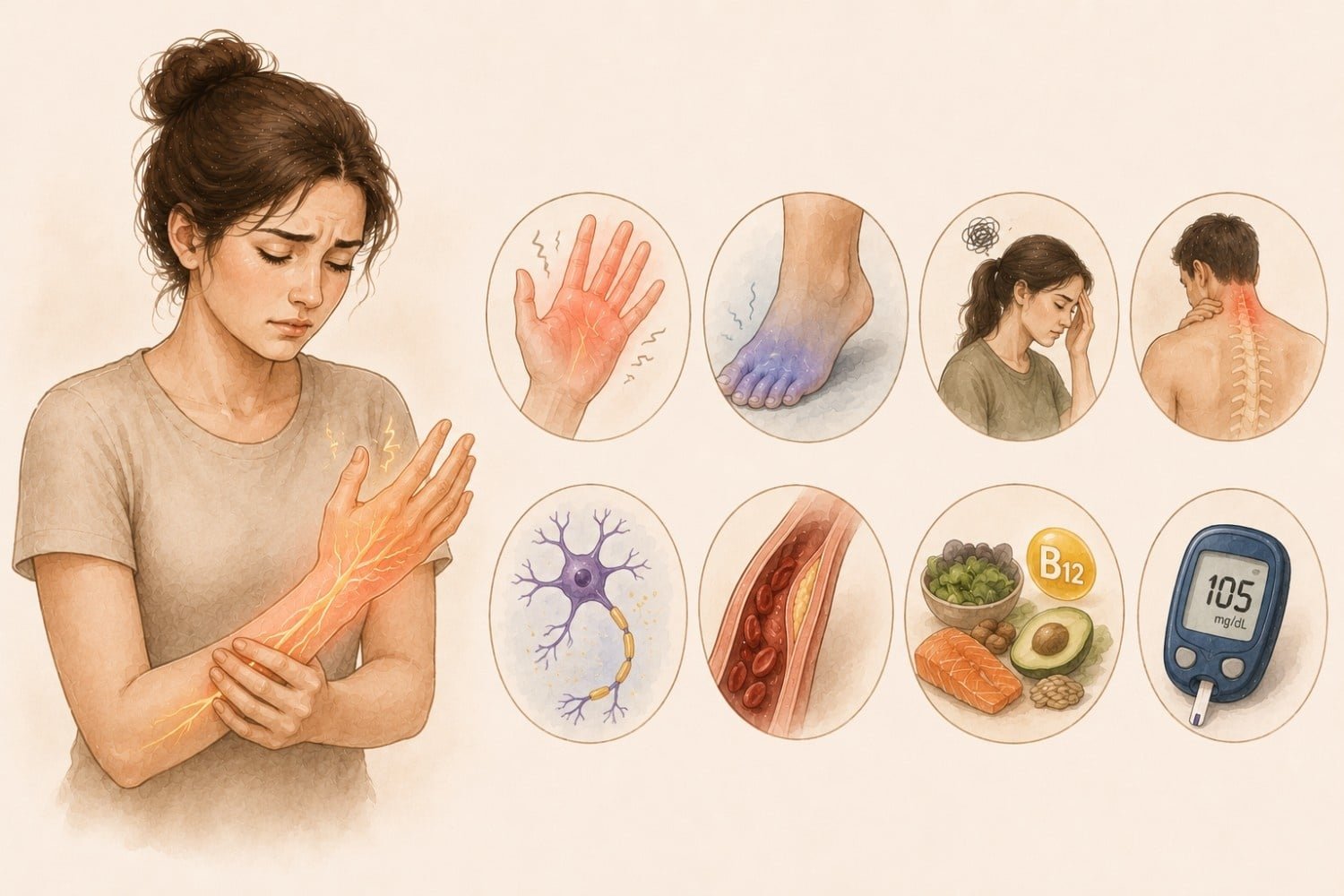
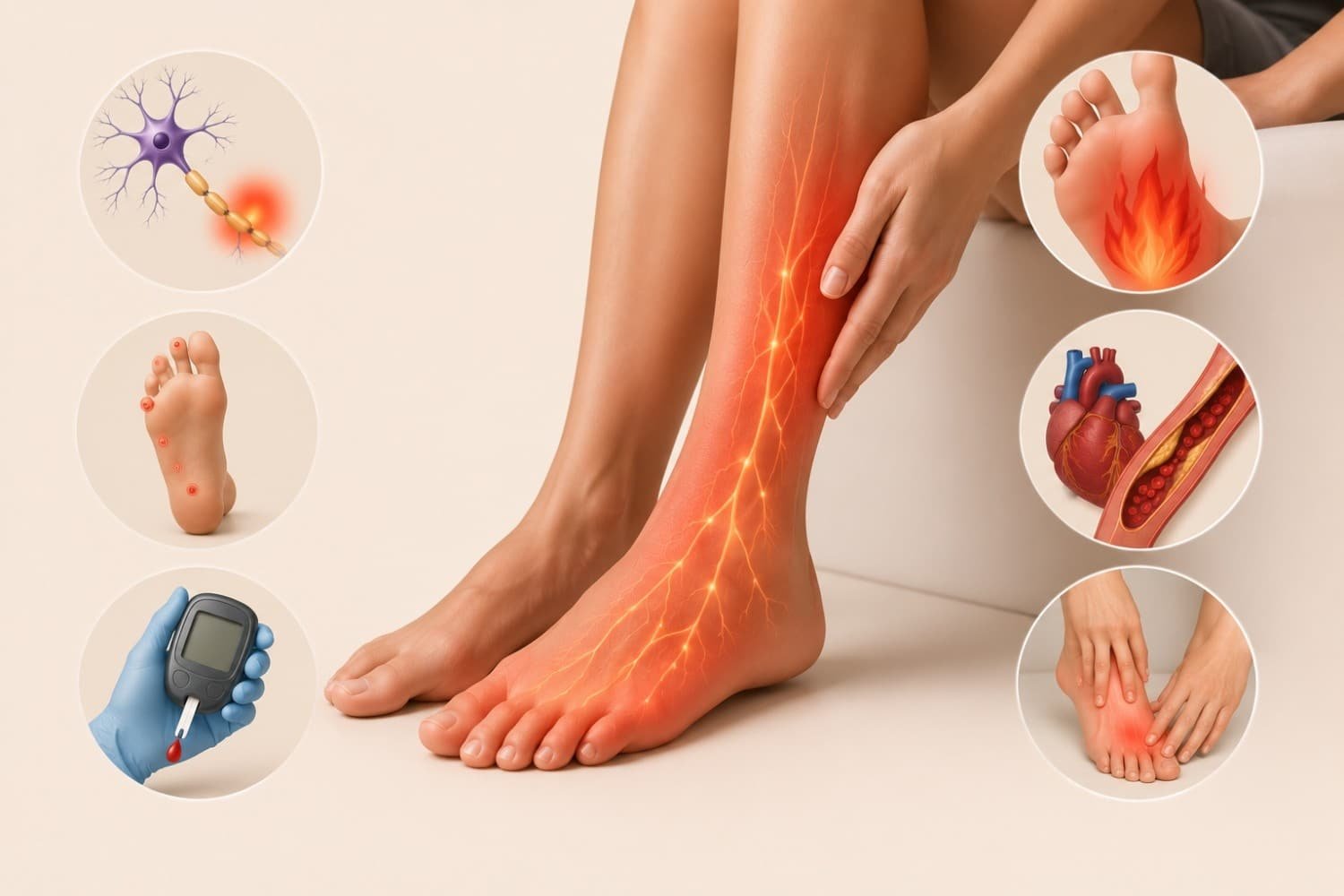
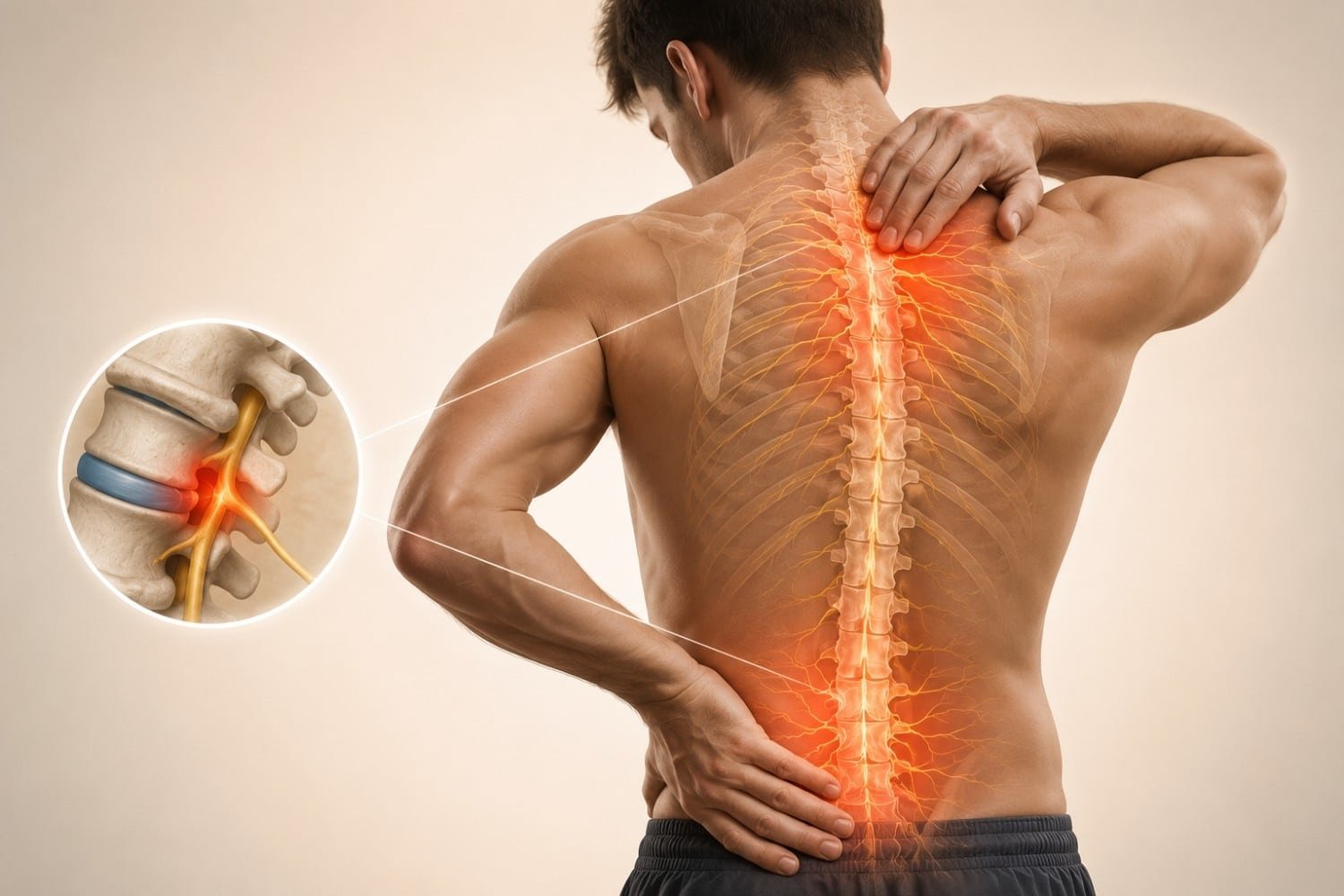
Have you ever had your foot fall asleep so deeply that walking felt like balancing on a cloud made of fizz? Or felt random tingling, prickling, or buzzing in your hands, face, or back for absolutely no reason? I’ve experienced both, and the first time it happened beyond the “I sat funny” moment, I genuinely wondered if my nervous system had decided to start a new hobby.
What I didn’t know back then is that there’s a medical name for all these strange sensations. It’s called paraesthesia. In this article, I’ll walk you through what paraesthesia really is, what causes it, how it’s diagnosed, and how to treat it. Everything I share here is grounded in trusted medical sources like the Mayo Clinic, Cleveland Clinic, the NHS, and the National Institute of Neurological Disorders and Stroke.
What Is Paraesthesia? A Clear Medical Definition
Paraesthesia is the medical term for abnormal sensations such as tingling, numbness, burning, prickling, buzzing, or pins and needles. These sensations occur when nerves are pressed, irritated, damaged, or misfiring.
Most people have experienced paraesthesia at least a few times in life. The familiar “my foot fell asleep” feeling is the simplest example. But paraesthesia can show up anywhere on the body, sometimes for short moments and sometimes long-term.
Understanding it helps you recognise when it’s harmless and when it deserves medical attention.
The Two Main Types of Paresthesia
There are two main types of paraesthesia, and they behave very differently.
Transient Paresthesia
This is the temporary type most people are familiar with. It comes from short-term nerve compression, like sitting cross-legged for too long or sleeping on your arm. It resolves once the pressure is relieved.
I personally get this every time I sit at a coffee shop for too long with my legs crossed. Five minutes of walking usually fixes it. Classic.
Chronic Paresthesia
This type is long-lasting and often signals an underlying medical condition. It can come from nerve damage, neurological disorders, diabetes, or deficiencies. Chronic paraesthesia requires evaluation since it usually points to a specific cause.
The American Academy of Neurology clearly distinguishes between transient and chronic paraesthesia because the treatment paths differ.
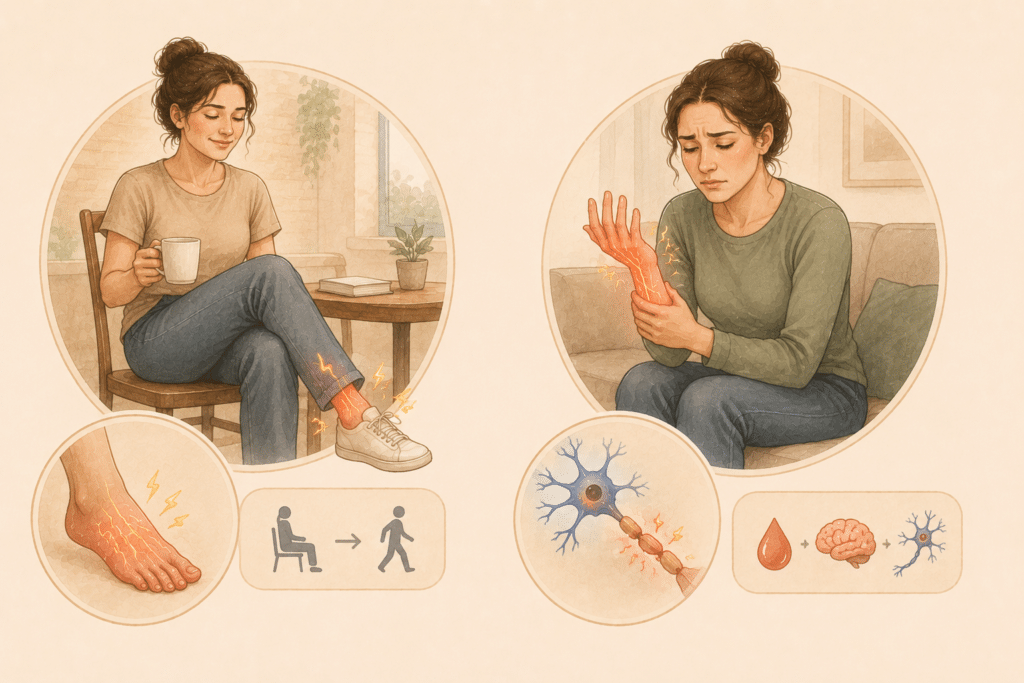
Common Symptoms of Paresthesia
Paraesthesia isn’t always just tingling. It includes a range of sensations, such as the following:
- Numbness
- Pins and needles
- Burning
- Buzzing
- Prickling
- Crawling skin (formication)
- Electric shock sensations
- Coldness or hotness without cause
- Light “fizzing” or fluttering
These sensations can appear anywhere, but they’re most common in the hands, feet, arms, legs, face, and scalp. I’ve personally felt almost all of these at some point, and the location often gives a strong clue about the cause.
Common Causes of Paresthesia
Let me walk you through the most common reasons behind paraesthesia, based on real-world experience and credible medical sources.
Nerve Compression
This is the most common cause overall. When a nerve gets compressed, even briefly, it sends abnormal signals. Conditions like carpal tunnel syndrome, sciatica, ulnar nerve compression, and pinched nerves in the neck or back are common examples.
I had a friend who blamed his random arm tingling on his backpack for weeks. Turned out his cervical posture was the real issue.
Diabetes (Diabetic Neuropathy)
Long-term high blood sugar damages tiny nerves, especially in the hands and feet. The CDC notes that nearly half of people with diabetes develop some form of neuropathy.
If you have diabetes and experience persistent tingling, burning, or numbness, blood sugar control becomes critical. Early intervention genuinely slows the damage.
Vitamin B12 Deficiency
Low B12 affects nerve health and is one of the most overlooked causes of paraesthesia. It’s especially common in vegetarians, older adults, and people on long-term acid reflux medications like omeprazole.
A simple blood test confirms it, and supplementation usually clears the symptoms.
Multiple Sclerosis (MS)
MS happens when the immune system damages the protective coating around nerves, leading to misfires that show up as tingling, numbness, or burning anywhere on the body.
The National MS Society recognises paraesthesia as one of the most common early symptoms. If your tingling comes with vision changes, fatigue, or balance issues, get evaluated by a neurologist.
Anxiety and Stress
Anxiety is a huge driver of paraesthesia. Hyperventilation, stress hormones, and an overactive nervous system make nerves hypersensitive. The result is random tingling, buzzing, or numb sensations across the body.
I’ve personally noticed mine spike during high-stress weeks. Once stress calms, the sensations fade.
Stroke or Transient Ischemic Attack (TIA)
This is rare but extremely important. Sudden paraesthesia on one side of the body, especially with weakness, slurred speech, or vision changes, can signal a stroke. Treat this as an emergency.
Peripheral Neuropathy
This refers to damage to nerves outside the brain and spinal cord. Causes range from diabetes to alcohol use, chemotherapy drugs, infections, and autoimmune diseases.
The symptoms often start in the feet and slowly move upward. They can include tingling, burning, numbness, and weakness.
Pregnancy
Fluid retention and pressure on nerves during pregnancy can cause paraesthesia, especially in the hands and feet. It usually resolves after delivery but is worth mentioning to a doctor.
Medications and Substances
Several medications, including chemotherapy drugs, certain antibiotics, antidepressants, and seizure medications, can cause paraesthesia. Alcohol and recreational drugs may also damage nerves over time.
Spinal Cord Issues
Conditions like spinal stenosis, herniated discs, or spinal cord injuries can cause paraesthesia in different parts of the body, depending on the affected area.
Infections
Some infections directly affect nerves, including shingles, Lyme disease, HIV, and certain viral infections. Paraesthesia is a common early symptom in many of these cases.
Where Paresthesia Happens and What the Location Tells You
The location often gives strong clues about the cause.
If the sensation is in your hands, think carpal tunnel, ulnar nerve compression, or cervical issues.
If it’s in your feet, peripheral neuropathy, diabetes, or sciatica are common causes.
If it’s on your face, anxiety, trigeminal nerve irritation, or migraine auras may be involved.
If it appears on the scalp or head, stress, occipital neuralgia, or sensory sensitivity often plays a role.
If the paraesthesia is one-sided, neurological causes like stroke or MS should be evaluated quickly.
If it shows up on both sides, systemic causes like diabetes or B12 deficiency are more likely.
This pattern-based thinking is exactly how neurologists narrow down causes during a clinical exam.
Red Flags You Should Never Ignore
Most paraesthesia is harmless and temporary, but some situations need urgent attention.
Please seek medical care immediately if your paraesthesia comes with the following:
- Sudden weakness
- Slurred speech
- Vision changes
- Facial drooping
- Severe headache
- Loss of bladder or bowel control
- Difficulty walking
- Numbness that spreads quickly
Trust your instincts. If something feels deeply off, don’t wait it out. Conditions like stroke, cauda equina syndrome, or severe nerve damage are time-sensitive.
How Doctors Diagnose Paresthesia
When I finally got mine properly evaluated, the process was thorough. Diagnosing paraesthesia isn’t guesswork.
A standard workup includes a detailed history, physical exam, and neurological assessment. Blood tests check for B12, blood sugar, thyroid function, and inflammation markers.
For nerve-related causes, nerve conduction studies and EMG help check nerve health. If the issue is suspected to be in the spine or brain, an MRI may be needed.
For chronic or unexplained paraesthesia, doctors may refer you to a neurologist for further testing. A proper diagnosis prevents months of guesswork and unnecessary treatment.
Treatment Options for Paresthesia
Treatment depends entirely on the cause, but here’s what generally works in real-world cases.
Lifestyle Adjustments
For mild cases, simple changes do a lot. Staying hydrated, eating balanced meals, getting consistent sleep, and improving posture often reduce symptoms significantly. I started taking short walking breaks every hour, and my random tingling episodes reduced sharply.
Addressing the Underlying Condition
If the cause is diabetes, blood sugar control is essential. If it’s a vitamin deficiency, supplementation usually clears it. MS, neuropathy, or spinal causes require targeted medical treatment.
In most cases, fixing the root cause stops the paraesthesia for good.
Medications
For nerve-related paraesthesia, doctors may prescribe gabapentin, pregabalin, or duloxetine. NSAIDs help with inflammation. Steroid injections are sometimes used for nerve compression.
Always use these under proper medical supervision.
Physical Therapy
A skilled physiotherapist can teach nerve gliding exercises, stretches, and posture corrections that genuinely reduce nerve irritation. This is especially helpful for carpal tunnel, sciatica, and cervical issues.
Stress and Anxiety Management
If anxiety is the trigger, slow breathing, mindfulness, regular exercise, and reducing caffeine help calm the nervous system. CBT is highly effective for anxiety-related paraesthesia.
I personally found that 10 minutes of slow breathing before bed reduced my random buzzing sensations significantly.
Surgery in Severe Cases
If conservative treatment fails, surgical options like carpal tunnel release, cubital tunnel decompression, or spinal decompression provide real relief. These are not first-line treatments but work well when nothing else does.

Living With Paraesthesia: Practical Tips
Paraesthesia: Many people live with chronic paraesthesia without it controlling their lives. Here are real-world strategies that genuinely help.
Try to maintain a consistent sleep routine, since fatigue worsens nerve symptoms. Stretch daily, especially the neck, lower back, and hands. Avoid long hours of sitting without movement. Stay hydrated and eat foods rich in B12, magnesium, and iron.
Identify your triggers. For some, it’s stress. For others, it’s posture or sleep position. Keeping a small symptom journal helps a lot, both for yourself and your doctor.
I’ve personally found that small lifestyle improvements often produce bigger results than any single medication.
Frequently Asked Questions
Most cases are harmless and temporary. Chronic or sudden paresthesia needs medical evaluation to identify the cause.
Yes. Stress and anxiety are major triggers because they overstimulate the nervous system and increase hyperventilation.
Temporary paresthesia lasts a few minutes. Chronic paresthesia can last weeks or months and usually has a specific cause.
If symptoms last more than a few days, spread, return often, or come with weakness or speech issues, get medical help.
Yes, often. Treating the underlying cause usually clears the symptoms. Some cases need long-term management.
Final Thoughts
Paraesthesia is one of those conditions that sounds dramatic but is usually very manageable once you understand what’s behind it. From nerve compression and deficiencies to anxiety and chronic conditions, the causes are wide, and so are the treatments.
If your body keeps acting like a malfunctioning Wi-Fi signal, don’t ignore it and don’t panic either. Track the patterns, fix the basics, and talk to a qualified doctor when needed. Your nervous system is constantly trying to communicate. The kindest thing you can do is finally listen.