Have you ever been sitting quietly, minding your own business, and suddenly felt a quick zap go through your body, like someone briefly plugged you into a low-voltage socket? I have, and I’ll be honest, the first time it happened, I genuinely paused mid-sip of my coffee and asked myself, “Did I imagine that?” Spoiler, I did not.
A sudden electric shock feeling in the body is more common than people think, and it almost always has a real explanation behind it. In this article, I’ll walk you through what it actually means, why it happens, and when it deserves urgent attention. Everything I’m sharing here is based on documented medical sources like the Mayo Clinic, Cleveland Clinic, and the National Institute of Neurological Disorders and Stroke.
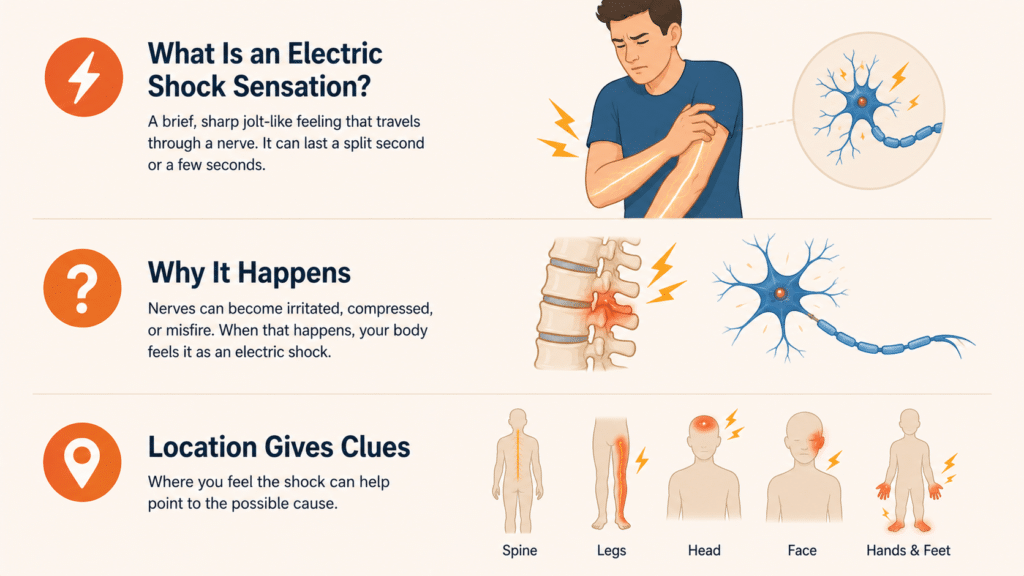
What Is an Electric Shock Sensation in the Body?
An electric shock sensation is a brief, sharp feeling that mimics a small jolt of electricity travelling through a nerve. It can last a fraction of a second or stretch into a few seconds. Some people feel it once a month, others several times a day.
The medical world calls these sensations “paresthesias“, but the electric-shock variety stands apart because of how sudden and sharp it feels. Unlike tingling or numbness, it has that unmistakable jolt-like quality that genuinely catches you off guard.
Why It Happens: The Simple Explanation
In most cases, an electric shock sensation means a nerve is being briefly irritated, compressed, or misfiring. Nerves carry electrical signals naturally, so when they get disturbed, the body interprets the disruption as, well, an actual shock.
The cause can be anything from a pinched nerve to a deficiency to something more neurological. The location of the sensation often gives the biggest clue, which I’ll cover later in this article.
10 Common Causes of Sudden Electric Shock Feelings in the Body
Let me walk you through the most common causes I’ve come across, both from real-life experience and from credible medical sources.
Lhermitte’s Sign
This is one of the most well-documented causes of electric shock sensations. Lhermitte’s sign happens when bending the neck forward triggers a brief, electric-like jolt running down the spine, sometimes into the arms or legs.
It’s commonly linked to multiple sclerosis but can also appear in vitamin B12 deficiency, cervical spine issues, or after radiation therapy to the neck. If your shocks happen specifically when you tilt your head, this is worth bringing up with a neurologist.
Multiple Sclerosis (MS)
MS is one of the more serious causes worth knowing about. It happens when the immune system damages the protective covering of nerves, leading to misfires that often feel like shocks, tingling, or burning.
According to the National MS Society, electric shock sensations are a recognised symptom, especially in early stages. They’re rarely the only symptom, though. MS usually comes with fatigue, vision changes, balance issues, or numbness.
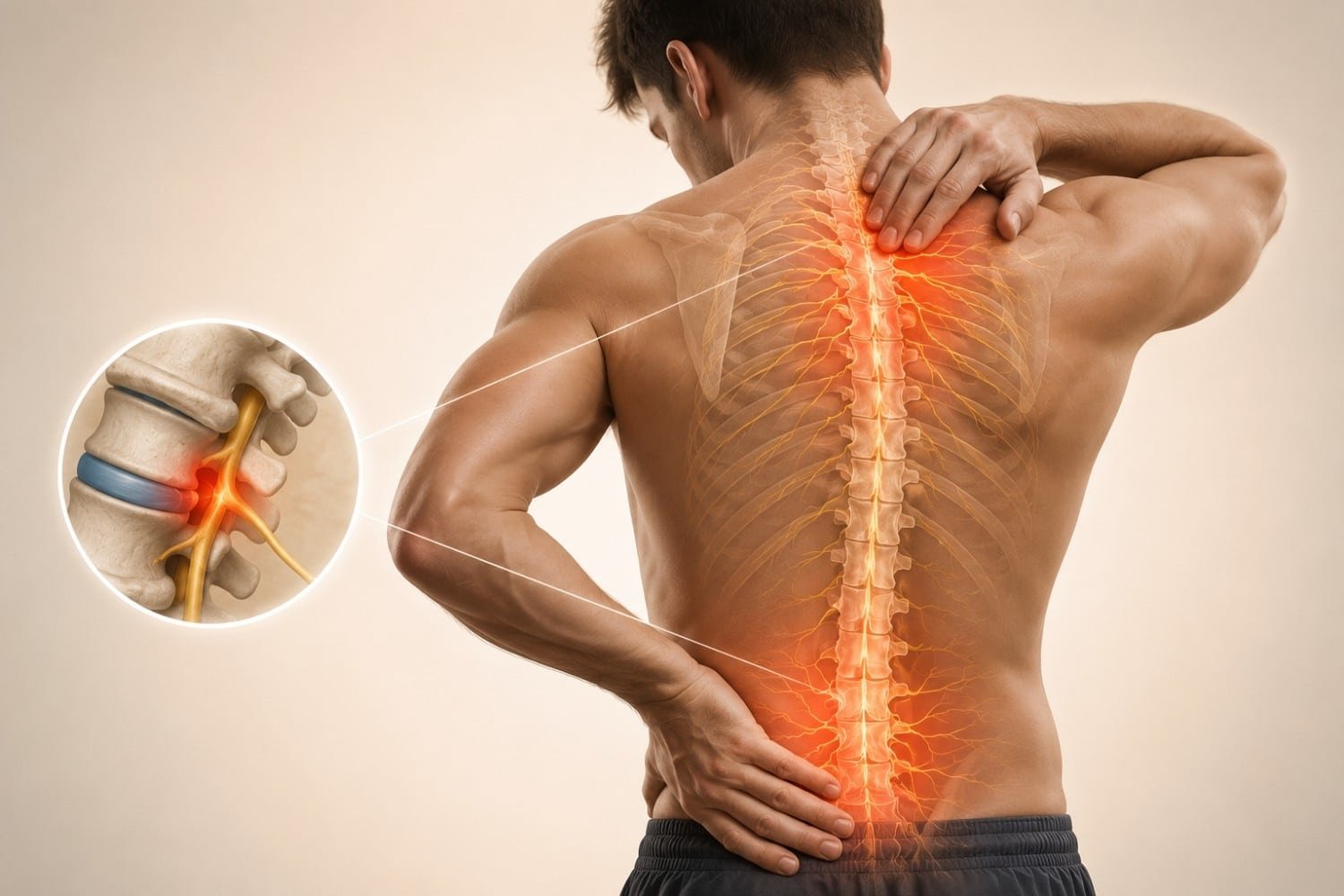
Pinched Nerves
A pinched nerve in the neck (cervical radiculopathy) or lower back (lumbar radiculopathy) can send sharp electric jolts through the arms or legs. Sciatica is the classic example, where the shock-like pain travels from the lower back down the leg.
I had a friend who described his sciatica perfectly: “It feels like someone is flicking a wire inside my leg.” Honestly, that captures it.
Vitamin B12 Deficiency
Low B12 affects the protective coating around nerves, which leads to all sorts of weird sensations, including electric shocks. It’s especially common in vegetarians, older adults, and people on long-term acid reflux medications like omeprazole.
A simple blood test confirms it, and treatment is usually as straightforward as supplementation or B12 injections. I’ve personally seen people feel completely different within a few weeks of fixing their levels.
Anxiety and Panic Attacks
Anxiety can absolutely cause electric shock sensations, even though it’s often dismissed. When the nervous system is stuck in fight-or-flight mode, nerves become hypersensitive and misfire easily.
These shocks are usually brief, random, and tend to appear during stressful weeks or panic episodes. If your jolts spike along with racing thoughts or chest tightness, anxiety might be a real factor.
Medication Withdrawal
This is a big one that doesn’t get talked about enough. Stopping certain antidepressants, especially SSRIs and SNRIs, can cause “brain zaps”, a well-documented withdrawal symptom that feels exactly like brief electric shocks in the head or body.
Cleveland Clinic and other reputable sources clearly recognise this. If you’ve recently reduced or stopped a medication, this could be the reason. Always taper under medical guidance.
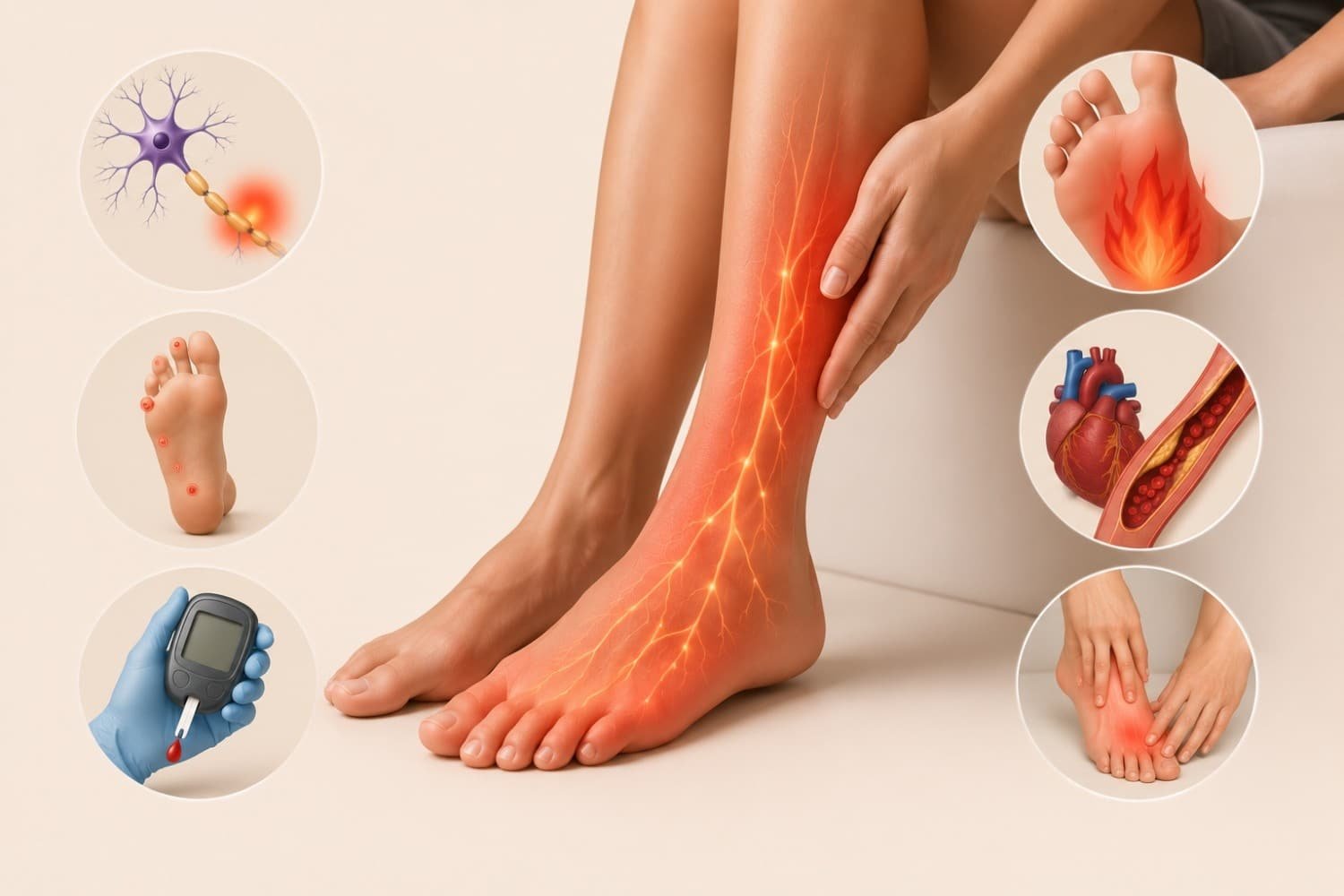
Diabetic Neuropathy
Long-term high blood sugar damages small nerves, especially in the hands and feet. The damage often produces electric shock sensations, burning, or tingling. The CDC notes that nearly half of people with diabetes develop nerve issues at some point.
Early blood sugar control genuinely slows the damage, which is why it’s worth taking these symptoms seriously.
Trigeminal Neuralgia
If the shock sensation hits your face, especially on one side, trigeminal neuralgia might be the culprit. It’s a nerve disorder that causes sudden, intense, electric-like facial pain triggered by simple actions like brushing teeth or chewing.
It’s painful but treatable, and a neurologist can confirm it through a clinical exam and imaging.
Shingles and Postherpetic Neuralgia
Shingles can leave behind nerve damage that produces electric shock sensations long after the rash clears. This condition, called postherpetic neuralgia, can last for months or even years if untreated.
If you’ve had shingles in the past and now feel random jolts in the same area, this is likely the cause.
Stress and Sleep Deprivation
A lesser-known but very real trigger. When the body is exhausted or under heavy stress, the nervous system becomes jumpy, leading to random misfires. I’ve felt these myself during back-to-back project deadlines, and once sleep returned to normal, so did my body.

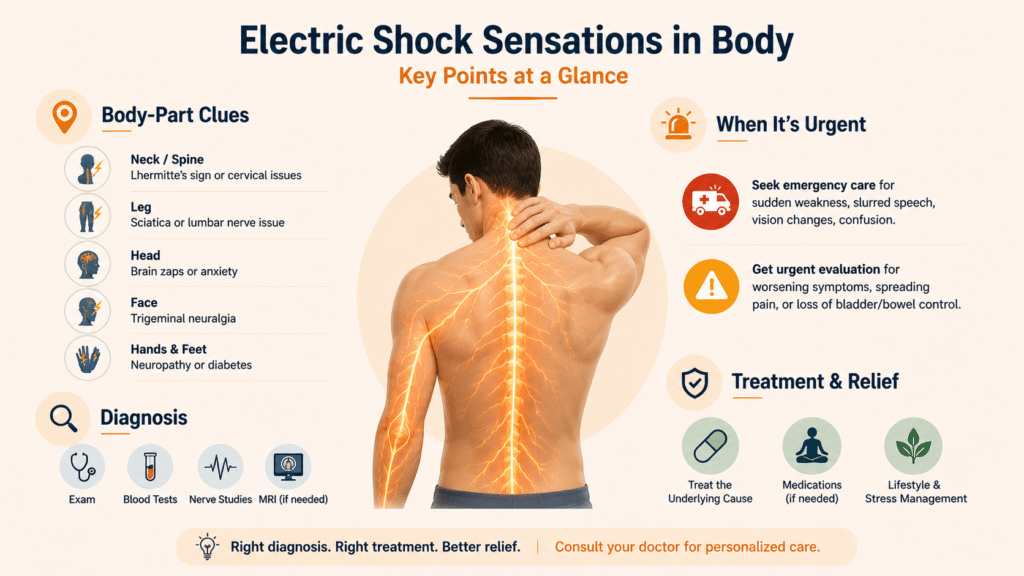
Body-Part Breakdown: What the Location Tells You
The location of the shock sensation can hint at the cause.
If the shock runs down the spine when bending your neck, think Lhermitte’s sign or cervical issues.
If it travels down one leg, sciatica or a lumbar nerve issue is the most likely cause.
If it appears in the head, brain zaps from medication withdrawal or anxiety often come into play.
If it shows up in the face, trigeminal neuralgia is worth ruling out.
If it hits the hands and feet repeatedly, peripheral neuropathy or diabetes-related nerve damage tops the list.
This pattern-based thinking is exactly how neurologists narrow down the cause during the first few minutes of an exam.
When the Sensation Is Urgent
Most electric shock sensations are harmless and easily explained. But some situations need immediate attention.
If the shock comes with sudden weakness, slurred speech, vision changes, confusion, or facial drooping, treat it as an emergency. These can be early signs of a stroke or serious neurological issue.
If the sensations are frequent, worsening, spreading, or paired with loss of bladder or bowel control, please don’t wait. Spinal cord problems are time-sensitive and need quick evaluation.
How Doctors Diagnose the Cause
When I finally went to a doctor about my own jolts years ago, I was surprised at how methodical the process was. Diagnosing electric shock sensations isn’t a guessing game.
A proper workup usually includes a neurological exam, blood tests for B12, blood sugar, thyroid function, and sometimes inflammation markers. Nerve conduction studies and EMG help check nerve health, while MRI scans of the spine or brain are useful when conditions like MS or pinched nerves are suspected.
The right diagnosis prevents months of trial-and-error treatments. It’s worth the time.
How to Treat and Reduce Electric Shock Sensations
Treatment depends entirely on the cause, but here’s what generally works in real-world cases.
Address the Underlying Condition
If the cause is B12 deficiency, supplementation often clears it. If it’s diabetes, blood sugar management is key. MS-related sensations respond to disease-modifying therapies prescribed by neurologists.
In most cases, fixing the root cause does more than treating the sensation directly.
Medication Options
Doctors may prescribe gabapentin, pregabalin, or duloxetine for nerve-related sensations. Carbamazepine is often used for trigeminal neuralgia. NSAIDs help when inflammation is part of the picture.
Self-medicating is a bad idea here. These medications need proper dosing and monitoring.
Lifestyle and Nutritional Support
Hydration, balanced meals, regular sleep, and stress management make a noticeable difference. I’ve seen people reduce their episodes drastically just by improving sleep and cutting caffeine.
Light exercise, stretching, and physiotherapy also help, especially when nerve compression is involved.
Reducing Anxiety-Driven Episodes
If anxiety is the trigger, slow breathing, therapy, mindfulness, and reducing stimulants like caffeine genuinely help. The nervous system calms down when given the right environment.
I personally found that just 10 minutes of slow breathing before bed cut my random episodes significantly.
Frequently Asked Questions
It’s usually a brief nerve misfire caused by anxiety, fatigue, B12 deficiency, or minor nerve compression. Most cases are harmless, but persistent ones need medical review.
Mildly, yes. Electrolyte imbalances from dehydration can make nerves more reactive, leading to random shocks.
Not typically. They’re most often linked to antidepressant withdrawal and ease over time, especially with proper tapering under medical supervision.
Occasional, brief shocks usually aren’t a concern. Worry only when they become frequent, spread, or appear with neurological symptoms.
Final Thoughts
A sudden electric-shock feeling in the body is unsettling, but it’s almost always your nervous system reacting to something specific. From Lhermitte’s sign and MS to anxiety, deficiencies, and medication withdrawal, the causes are varied, and so are the treatments.
If your jolts keep showing up, don’t ignore them and don’t panic either. Track the pattern, note the triggers, and talk to a qualified doctor. Your body is sending a signal, sometimes politely, sometimes loudly. Either way, it’s worth listening.