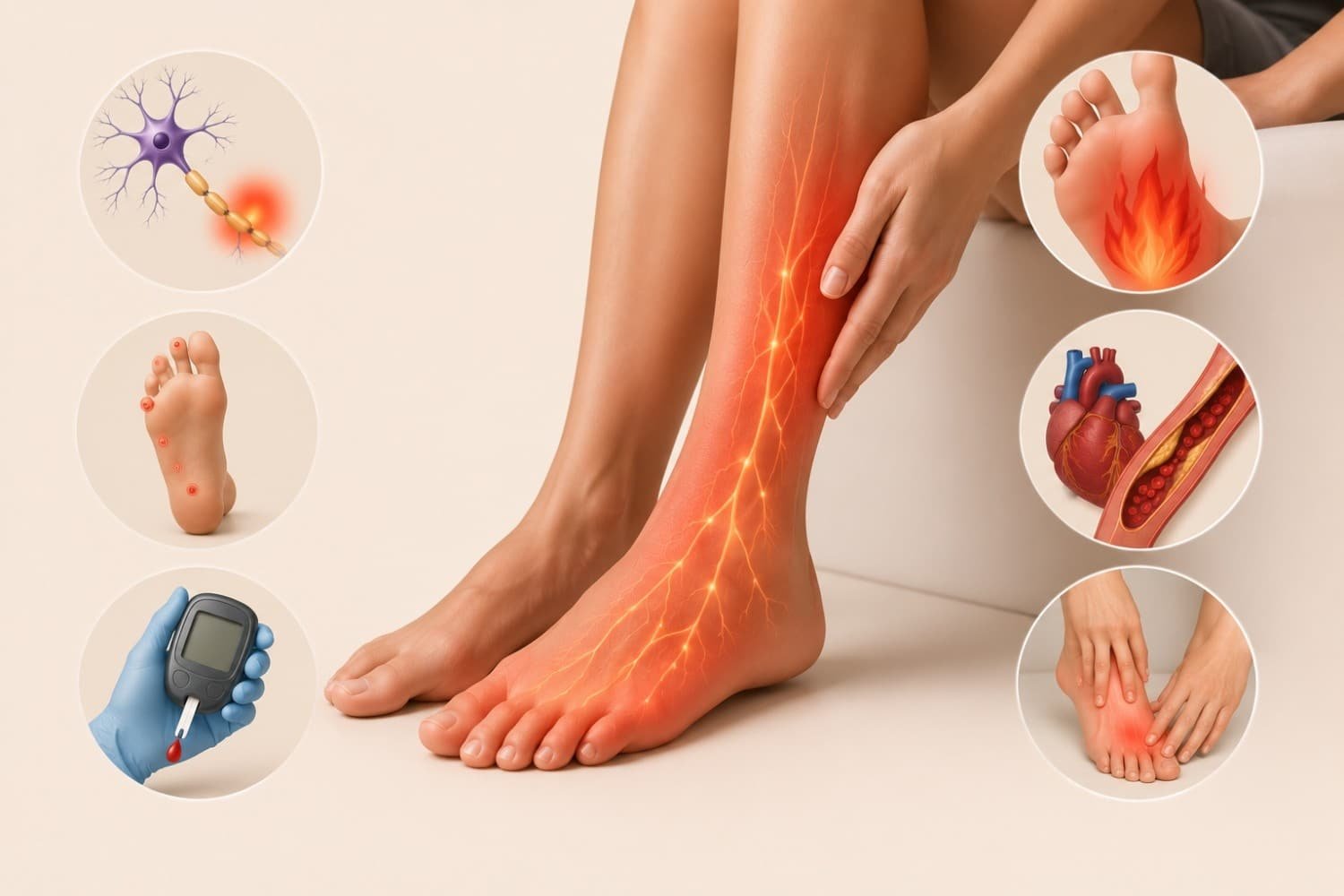
Have you ever sat cross-legged for too long and suddenly felt your foot turn into a buzzing, prickly stranger that refuses to cooperate? Yeah, I’ve been there too. That weird, tingling sensation we casually call “pins and needles” is something almost every human on the planet has experienced at some point. It’s annoying, sometimes funny, and occasionally a little alarming.
In this article, I’ll walk you through everything I’ve learned about this strange sensation, from why it happens to when you should actually start worrying about it. I’ve spent a fair amount of time researching neurology basics, talking to people who deal with chronic versions of this, and digging through trusted medical sources to put this together. So let’s get into it.
What Is the Pins and Needles Sensation?
The medical term for this feeling is paresthesia. I know, it sounds fancier than it deserves to. Paresthesia refers to that tingling, prickling, burning, or “asleep” feeling in your skin, usually without any obvious physical cause like an injury.
According to the National Institute of Neurological Disorders and Stroke (NINDS), paresthesia happens when there’s pressure on a nerve or when nerve signals get temporarily disrupted. Most of us experience the temporary kind, which fades within a few minutes.
But there’s also a chronic form, and that one usually points to an underlying issue. I’ll get into that shortly.
Why Does Pins and Needles Happen?
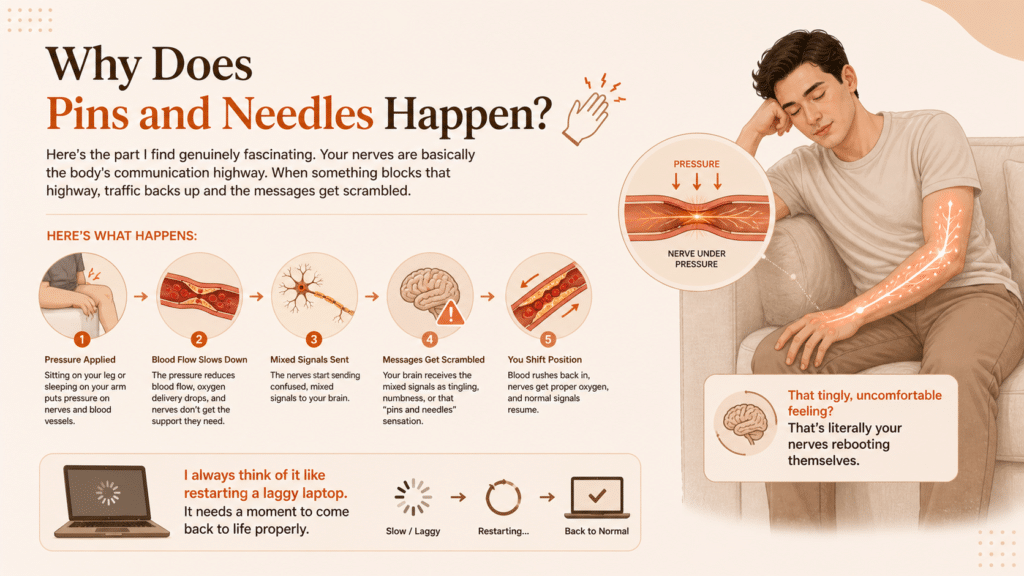
Here’s the part I find genuinely fascinating. Your nerves are basically the body’s communication highway. When something blocks that highway, traffic backs up and the messages get scrambled.
When you sit on your leg or sleep on your arm, you’re putting pressure on nerves and blood vessels. The blood flow slows down, oxygen delivery drops, and the nerves start sending mixed signals to your brain. Once you shift position, blood rushes back in, and your nerves wake up. That uncomfortable, tingly feeling? That’s literally your nerves rebooting themselves.
I always think of it like restarting a laggy laptop. It needs a moment to come back to life properly.
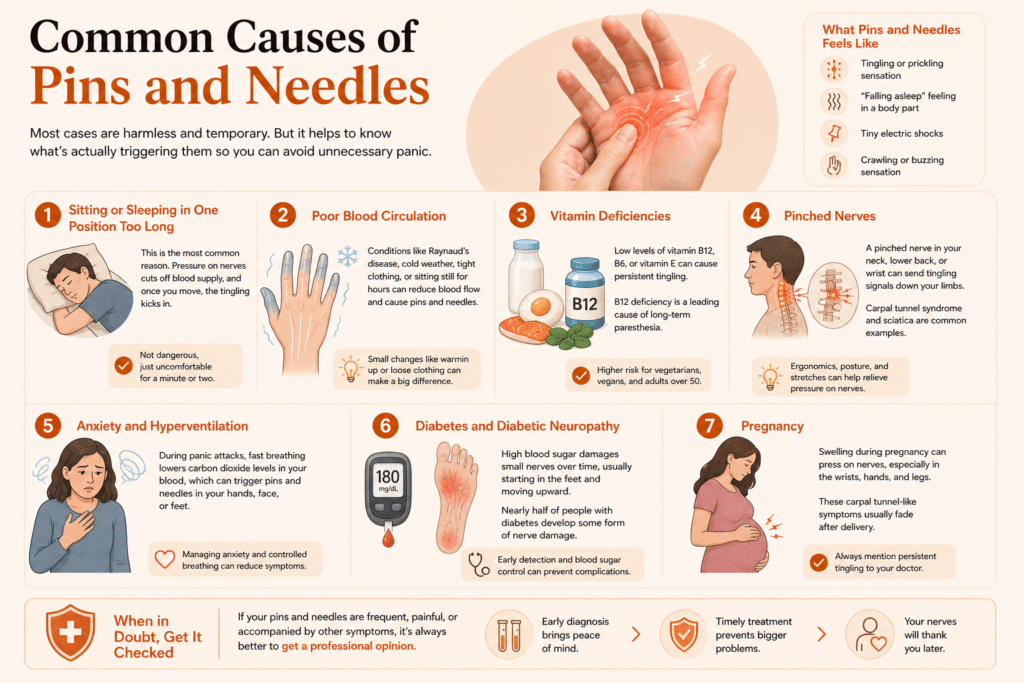
Common Causes of Pins and Needles
Most cases are harmless and temporary. But it helps to know what’s actually triggering them so you can avoid unnecessary panic.
1. Sitting or Sleeping in One Position Too Long
This is the most common reason. If you’ve ever woken up with a “dead” arm because you slept on it, you know exactly what I mean. The pressure cuts off blood supply to the nerves, and once you move, the tingling kicks in.
It’s not dangerous, just uncomfortable for a minute or two.
2. Poor Blood Circulation
Sometimes circulation issues, like Raynaud’s disease, cause pins and needles, especially in fingers and toes. Cold weather, tight clothing, or sitting still for hours can all affect blood flow.
I once spent an entire winter wondering why my toes felt weird in the morning. Turns out, my socks were way too tight. Lesson learned.
3. Vitamin Deficiencies
This one surprises a lot of people. A deficiency in vitamin B12, B6, or vitamin E can cause persistent tingling. The Mayo Clinic and Cleveland Clinic both list B12 deficiency as a leading cause of long-term paresthesia.
If you’re vegetarian, vegan, or over the age of 50, your risk is slightly higher because B12 mostly comes from animal sources or supplements.
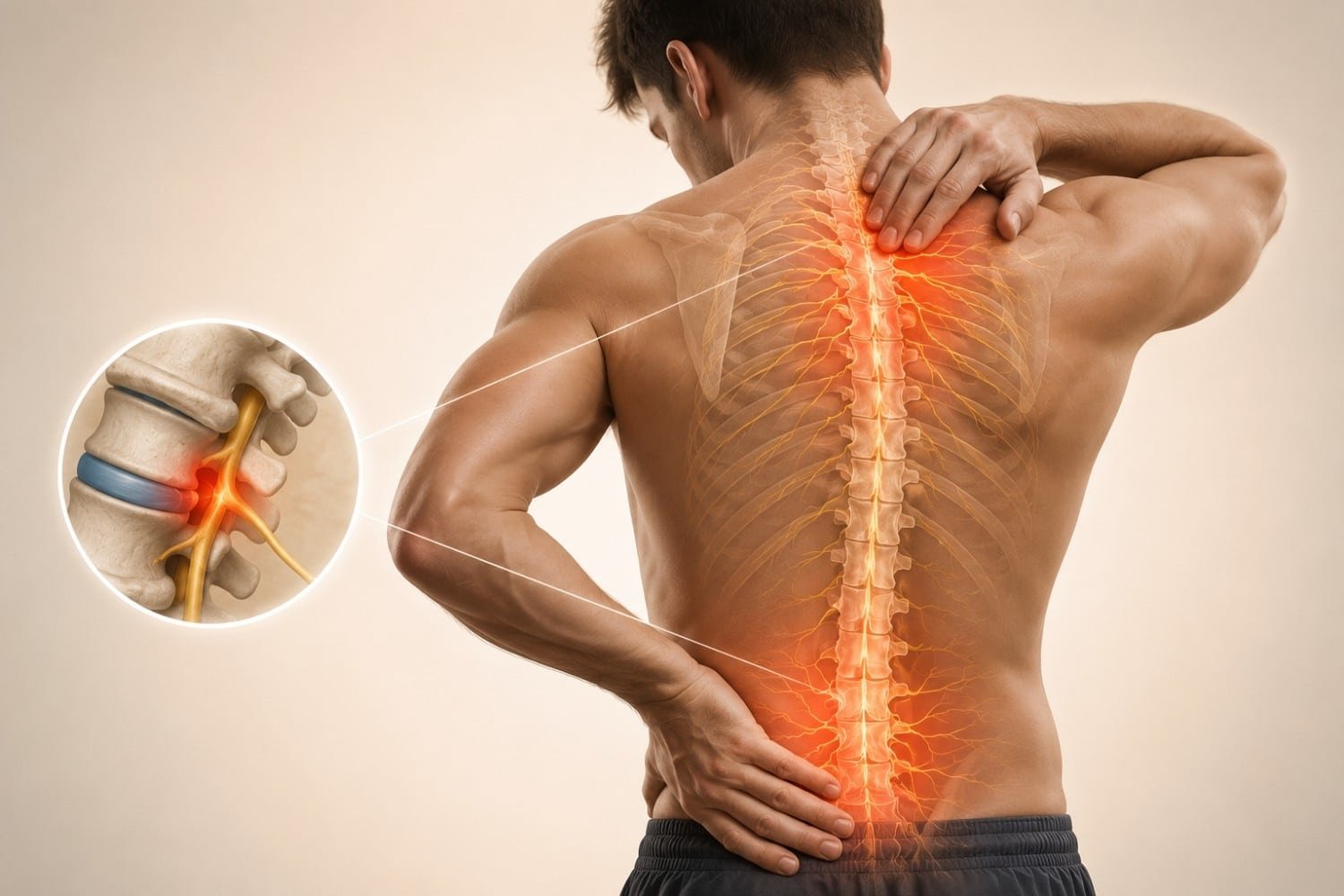
4. Pinched Nerves
A pinched nerve in your neck, lower back, or wrist can send tingling signals down your limbs. Conditions like carpal tunnel syndrome and sciatica are classic examples.
I’ve personally seen friends struggle with carpal tunnel after months of laptop use without proper wrist support. It’s more common than people think, especially in remote workers.
5. Anxiety and Hyperventilation
Yes, anxiety can absolutely cause pins and needles. When you breathe too quickly during a panic attack, the carbon dioxide levels in your blood drop, and that affects nerve function.
I’ve spoken to people who genuinely thought they were having a stroke during their first panic attack because of how intense the tingling was. Knowing this can save someone a lot of fear.
6. Diabetes and Diabetic Neuropathy
Long-term high blood sugar damages small nerves over time. This is called diabetic neuropathy, and it usually starts in the feet before moving upward.
The American Diabetes Association notes that nearly half of people with diabetes develop some form of nerve damage. So if someone has diabetes and starts feeling persistent tingling, it’s worth a doctor’s visit.
7. Pregnancy
During pregnancy, swelling can press against nerves, especially in the wrists, hands, and legs. This is why a lot of pregnant women develop carpal tunnel-like symptoms.
It usually fades after delivery, but it’s worth mentioning to a doctor anyway.
When Pins and Needles Become Serious
Now this is where I want you to pay close attention. Most cases are harmless. But there are red flags that should never be ignored.
You should consult a doctor immediately if you experience pins and needles along with:
- Sudden weakness on one side of the body
- Slurred speech or confusion
- Severe headache
- Loss of bladder or bowel control
- Tingling that doesn’t go away after hours or days
- Tingling that spreads rapidly across your body
These symptoms could indicate a stroke, multiple sclerosis, a serious nerve injury, or another neurological condition. I’m not trying to scare anyone, but knowing the warning signs genuinely matters.
Body Parts Most Affected by Pins and Needles
The sensation can show up almost anywhere, but some areas are more prone to it than others.
Hands and Fingers
Carpal tunnel syndrome, repetitive strain, or sleeping with your hand under your pillow are common culprits. If you work long hours on a computer, this is something to keep an eye on.
Feet and Toes
Diabetic neuropathy, vitamin deficiencies, and tight footwear are usually behind tingling in the feet. I’ve also noticed that long-distance runners sometimes deal with this temporarily.
Legs
Sciatica is a top reason for tingling that runs from the lower back down through the leg. It’s often described as electric or burning, and it can make sitting unbearable.
Arms
Pinched nerves in the neck or shoulder can send tingling into the arms. Side sleepers tend to experience this more often.
Face
Facial paresthesia is less common, but it can happen due to migraines, dental issues, or in rare cases, neurological problems. If your face goes numb suddenly, please don’t ignore it.
How Pins and Needles Are Diagnosed
When you visit a doctor, they usually start with a physical exam and a few simple questions. They want to know how long it’s lasted, what makes it worse, and whether other symptoms are present.
If they suspect something deeper, they may order:
- Blood tests to check vitamin levels and blood sugar
- Nerve conduction studies to see how well your nerves transmit signals
- MRI or CT scans to look for pinched nerves or spinal issues
- Electromyography (EMG) to evaluate muscle and nerve health
I’ve found that diagnosis can be a bit of a process. Don’t get frustrated if it takes more than one visit to figure things out.
Treatment Options for Pins and Needles
Treatment really depends on the cause. There’s no one-size-fits-all fix, and anyone telling you otherwise probably hasn’t dealt with it themselves.
Lifestyle Adjustments
For temporary cases, the fix is simple. Move around, change positions, and avoid sitting cross-legged for an entire movie marathon. Trust me, your legs will thank you.
If you’re someone who works long hours at a desk, ergonomic furniture and proper posture make a noticeable difference. I started using a wrist rest a couple of years ago and the difference was immediate.
Nutritional Support
If a vitamin deficiency is the cause, supplementation usually helps. B12 injections or oral supplements are commonly prescribed. Always check with a doctor before starting supplements, since taking too much of certain vitamins can cause issues too.
Physical Therapy
For pinched nerves, sciatica, or carpal tunnel, physical therapy can be a game changer. Targeted stretches and strengthening exercises help relieve nerve pressure naturally.
I’ve personally seen friends recover from sciatica with consistent physiotherapy, no surgery needed.
Medications
Doctors sometimes prescribe medications like gabapentin, pregabalin, or certain antidepressants for chronic nerve pain. These don’t fix the cause but help manage symptoms.
Treating Underlying Conditions
If diabetes, multiple sclerosis, thyroid issues, or another condition is the root cause, treating that condition is the priority. Once the underlying issue is managed, the tingling often improves.
Home Remedies
Some people find relief with warm compresses, gentle massage, or even yoga. While these aren’t cures, they can ease mild cases. Just don’t rely on home remedies if symptoms persist or worsen.
How to Prevent Pins and Needles
Prevention isn’t always possible, but a few habits genuinely help.
Stay active, keep your blood sugar in check, eat a balanced diet rich in B vitamins, take breaks during long work hours, and avoid putting prolonged pressure on any one limb.
I’ve noticed that even small changes, like adjusting your sleeping position or switching to a better office chair, can reduce these episodes significantly.
Frequently Asked Questions
Is pins and needles dangerous?
Most of the time, no. It’s a temporary nerve reaction. But if it’s persistent, spreading, or paired with other symptoms, get it checked out.
Can stress cause pins and needles?
Absolutely. Stress and anxiety can trigger hyperventilation, which leads to tingling in the hands, face, and feet.
How long does pins and needles last?
Temporary cases fade within minutes. Chronic ones can last hours, days, or longer, depending on the cause.
Can dehydration cause tingling?
Yes, dehydration can disrupt electrolyte balance, which affects nerve signaling. Drink water consistently throughout the day.
Should I see a doctor for occasional pins and needles?
If it happens occasionally and goes away quickly, probably not. If it becomes frequent or severe, definitely yes.
Final Thoughts
Pins and needles is one of those sensations that we all brush off as harmless, and most of the time, it really is. But it can also be your body’s way of telling you something needs attention, whether it’s a vitamin deficiency, a pinched nerve, or something more serious.
The key is to listen to your body without panicking over every tingle. Pay attention to how often it happens, where it shows up, and whether other symptoms come along with it.
If you’re ever unsure, talking to a doctor is always the smarter move. Your nerves do a lot of quiet work for you every single day. The least we can do is take their occasional complaints seriously.